Hand, mouth and foot disease
introduction
Hand, mouth and foot disease is a common infectious disease that is caused by viral pathogens. Sometimes it is also called hand, foot and mouth rash or "false foot and mouth disease". It should not be confused with the true foot-and-mouth disease, which is also a highly contagious disease, but mainly occurs in cattle and pigs.
Symptoms
In hand, mouth and foot disease, there are both specific symptoms by which the disease can be recognized, as well as a number of rather unspecific and quite general symptoms.
After the incubation period The first symptoms appear from three to ten days, which are mainly expressed in the form of fever, low appetite to complete loss of appetite, sore throat and body aches as well as new headaches. In most cases about one to two days after the onset of the fever, the skin changes that are very specific for hand, mouth and foot disease develop.
Painful ones develop especially in the area of the oral mucosa Exanthema (Rashes). These appear in the form of small red spots, which usually develop into blisters and ultimately into canker sores. Aphthae are open spots in the mucous membrane that are caused by damage and are very painful. The tongue and gums can also be affected before canker sores develop. This can be very painful, especially when eating and drinking.
Read more information under Red spots on the tongue
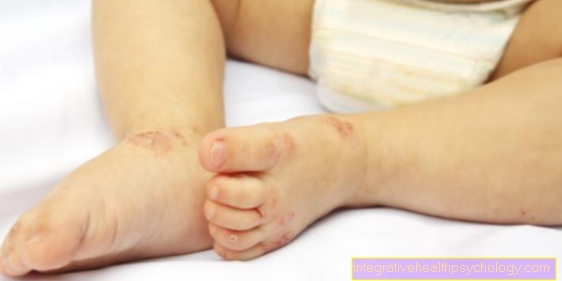
In addition to the changes in the mucous membrane in the mouth area, the very typical skin changes occur in the area of the palms of the hands and the soles of the feet
See also Rash on the foot
There, non-itchy, reddish-colored small nodules form, which can be either flat or raised (higher than the surrounding skin level). In addition, vesicles can develop there that are surrounded by a red border.
Read more on the topic:
- Blistered rash
- Rash on the sole of the foot
In addition to the soles of the feet and palms, the buttocks, genitals, squats and elbows can also be affected. The disease progression of hand, mouth and foot disease is usually rather mild, so that the disease resolves on its own within seven to ten days without any treatment.
In contrast to adults, children are usually more affected by the disease, as the symptoms are more pronounced. The disease usually heals without consequences.
fever
Hand, mouth and foot disease usually begins as a classic flu-like infection and includes a fever in almost everyone who is sick. Fever is a natural defense reaction of the body and shows that the immune system is working. A mild fever does not necessarily have to be lowered. At higher temperatures, which approach the 40-degree mark, antipyretic agents should be taken.
Furthermore, the increased fluid requirement should be taken into account in the case of fever. A guideline is that one liter more should be drunk for each additional degree.
Rash on the bottom
During hand, mouth and foot disease, a rash with small blisters forms in many parts of the body. In most cases it is located on the hands, the soles of the feet and in the mouth, giving it its name. With atypical courses, however, the bottom can also be affected. The rash is usually not itchy, but in exceptional cases it can be very itchy. If the rash is itchy, a soothing ointment on the bottom can help.
Rash on the tongue
The first signs that it is a hand, mouth and foot disease and not a flu-like infection are rashes in the mouth. Red spots and blisters form on the tongue, which can be very painful.
Some blisters develop into small sores called ulcers. In addition to the tongue, this rash also affects the lining of the mouth and gums. The disease usually heals completely within a few days without medical help and the rash on the tongue recedes.
Symptoms in adults
In the majority of adults, infections are completely symptom-free. However, these are still contagious to other people, especially children. When the disease breaks out in adults, it is very similar to the symptoms that occur in children.
The disease usually starts with a fever, sore throat and loss of appetite and is therefore easily mistaken for a classic cold. After two days, people will develop a rash around the mouth.
Red spots and blisters form on the tongue, gums and oral mucosa, which can also turn into ulcers. This rash is very painful. After a few days, a non-itchy rash forms on the hands and soles of the feet, which gives the disease its name. This rash can appear atypically in other parts of the body and it can also be very itchy.
Severe courses with meningitis or paralysis are very rare in both adults and children. Meningitis can manifest itself through a painfully stiff neck and those affected also appear dull and cloudy. Also in rare cases, fingernails and toenails can be lost after four weeks. However, this is a rather atypical course.
Symptoms during the incubation period
The incubation period is defined as the period after contact with the virus until the first signs of disease appear. Accordingly, no symptoms occur during the incubation period. However, it is possible that there is another disease that shows up during this time. However, this has nothing to do with the hand, mouth and foot disease virus. The incubation period usually lasts three to ten days. However, cases between one and 30 days have also been observed.
What is the course of hand-mouth-foot disease?
The illness usually begins like a typical cold. Those affected develop a fever and a sore throat, and loss of appetite. A general feeling of illness occurs.
On the second day, those affected complain of pain in the mouth. These are caused by a blotchy red rash with blisters that shows up on the tongue, the lining of the mouth and the gums. Some of these blisters can develop into small sores called ulcers, making the pain worse. One or two days later, a vesicular rash develops on the hands and soles of the feet, which, however, is mostly painless and does not itch. The rash can affect other parts of the body. Rashes in the hollow of the knees, elbows, buttocks and genital area are relatively common.
The condition usually clears up in about a week without medical attention. There is a risk of infection during the entire illness and sometimes for a few weeks afterwards. Severe courses are very rare and can include meningitis or paralysis.
therapy
There are no specific therapy in the treatment of hand, mouth and foot disease.
Because the disease mostly very mild runs, can only treated symptomatically for example, to treat the pain caused by eating and drinking from the wounds in the mouth.
There are no regular vaccines to prevent hand, mouth and foot disease.
However, vaccines are currently being developed for the West Pacific region, primarily to prevent the development of the enterovirus 71 disease.
Home remedies
Since no specific therapy is possible, those affected can only alleviate the symptoms. This can also be achieved with traditional home remedies. Cold compresses can help against the fever as they lower the body temperature.
Soothing teas, such as chamomile, can help against the sore throat. Home remedies can also be used for an itchy rash. Quark, for example, can have a cooling and calming effect on the skin. However, if you have a high fever, you should see a doctor.
homeopathy
Since there is no specific therapy for hand, mouth and foot disease, many parents want to try homeopathic treatment. The following means are recommended on relevant websites. The Globulis Mercurius Solubilis are said to relieve pain in the mouth and stimulate saliva production. Antimonium tartaricum is said to lower the fever. Borax is said to improve the sore throat. In the case of severe pain or high fever, however, a doctor should always be consulted who can help the child with medication.
forecast
The prognosis for hand, mouth and foot disease is in most cases very positive, as the disease is very mild.
Often the infected person does not even know that they have become infected with the pathogen, since the disease in adulthood can even run completely without symptoms, also known as asymptomatic.
Duration
Hand, mouth and foot disease is a typical viral disease that occurs particularly in childhood. After contact with the virus, it takes about three to ten days for the disease to begin.
From the onset of a fever, the illness usually lasts a week and heals without medical attention. Within that week, those affected are highly contagious. Even weeks after the actual illness, those affected can still be contagious, as the virus continues to be excreted. Long and severe courses are very rare and occur particularly in a virus strain that is widespread in Asia.
complication
In very rare cases there are complications. This can lead to meningitis (meningitis), as well as inflammation of the brain tissue (encephalitis). There may be polio-like paralysis of the arms and legs. After a while, the fingernails and toenails can also be lost.
Nails peel off
In very rare cases, hand, mouth and foot disease can lead to complications and atypical courses. A complication can be the loss of fingernails and toenails. These peel off after about four weeks. However, the nails grow back without any problems and no special therapy is required.
How long is there a risk of infection?
In the first week of the disease, the sick people or children are highly contagious. Even after the symptoms have subsided, those affected can remain infectious for a few more weeks, as the virus is excreted in the stool.
Risk of infection for infants
For infants, there are two ways in which hand, mouth and foot infection can develop. Women who show signs of hand, mouth and foot disease shortly before birth can transmit the virus to the newborn child during birth. Unlike some other infectious diseases, however, this does not mean that the course is more severe than with later infection.
However, the main risk of infecting an infant is older siblings.Infants often have no closer contact with other children with the exception of their own siblings, who can bring the virus with them from kindergarten or school. The highest risk of infection is during the first week and thus in the main phase of the disease.
Children who have hand, mouth and foot disease should therefore not be in direct contact with the infant. Since infection via contaminated surfaces is also possible, absolute protection in the home environment is almost impossible.
In addition to the obviously ill children, who are a source of infection, there are many infected people without symptoms. This means that the parents can also be carriers and show no signs of disease themselves. Good hand hygiene can at least reduce the risk. In most cases, even infants show a harmless course. Systemic complications are very rare and minimally more likely in the first two weeks of life.
How often can you get the disease?
After suffering from illness with a certain virus, there is lifelong immunity. However, this does not mean that hand, mouth and foot disease cannot recur. There are many different strains and subspecies of viruses that cause hand, mouth and foot disease, and immunity only exists against one pathogen.
Reinfection in kindergarten after a few weeks is rare, however, since in most cases all children carry the same strain of pathogen. It is also possible to vaccinate against a dangerous sub-type from South-East Asia if longer stays are planned there.
prophylaxis
There is one against hand, mouth and foot disease no vaccination as for other childhood diseases such as measles, mumps or rubella.
The most important thing about hand, mouth and foot disease infection is one good hand disinfection. This should regularly and really careful done as the hand, mouth and foot disease is one high risk of infection brings with it.
After every use of the toilet and change after each diaper In the case of a sick child, the hands should be washed properly with soap and also disinfected with a disinfectant.
Close contact with a child or adult with hand, mouth and foot disease should be avoided. Kissing, hugging, close cuddling or drinking from the same glass should also be avoided, as the virus is mainly transmitted via body fluids such as saliva.
diagnosis
The diagnosis of hand, mouth and foot disease is primarily made clinically.
The disease manifests itself through its typical skin symptoms on the palms of the hands and feet, so that the diagnosis can already be made based on its occurrence. This means that a laboratory test is usually superfluous.
The very mild course of the disease in most cases means that laboratory diagnostics are often not necessary. However, if you want to detect the pathogen, there is a quick diagnosis. This is available in the form of a so-called Enterovirus PCRwith which one can detect the specific RNA of the enteroviruses. It is also possible to detect the enteroviruses in stool samples, a throat swab or from the contents of the vesicles.
If the hand-mouth-foot disease does develop more severely with involvement of the nervous system, it is also possible to obtain nerve water (medicinally liquor) by means of a so-called lumbar puncture and to test this for the presence of enteroviruses.
In terms of differential diagnosis, the inflammatory ulcers that have developed in the oral cavity and the skin rash must be thought of as a number of other diseases. An alternative for the rash that occurs is chickenpox.
However, these affect not only the palms and feet, but the entire body.
With chickenpox, different stages of the disease occur at the same time. In addition to fresh vesicles, vesicles that have already burst and crusted can also be found on the body.
Some diseases can also lead to inflammatory ulcers in the area of the oral mucosa. In addition to hand-mouth-foot disease, so-called "mouth rot" (aphthous stomatitis), a herpes infection and also the real foot and mouth disease cause similar complaints.
root cause
Hand, mouth and foot disease is caused by viruses. Various pathogens come into question, but they all belong to the group of so-called "human enteroviruses"Belong. They are mainly infected in the summer and autumn months, but in contrast to some other pathogens, they are also very widespread in the environment.
Enteroviruses mainly colonize the human intestine. Hand, mouth and foot disease is caused by a number of different enteroviruses, all of which are from group A of the enteroviruses. These include Coxsackie A viruses and Coxsackie B viruses and the enteroviruses 71 as well as the so-called ECHO viruses.
The Coxsackie A and B viruses also have different subclasses. Coxsackie A16, but also A6, play an important role in hand-mouth-foot disease. In the B group, it is mainly Coxsackie B2 and B5 that are important. It is also interesting that the enteroviruses belong to the picornavirus family and, unlike humans, store their genetic material in the form of RNA.
Various models of infection can be considered as the causes of hand, mouth and foot disease. One possibility is the so-called fecal-oral transmission, i.e. the transmission of pathogens through stool excretion. Enteroviruses can still be detected in the stool after the symptoms have subsided after several weeks and there is a risk of infection.
Another way to get infected with hand, mouth and foot disease is that Droplet infection about coughing, sneezing and or kissing. Another possibility is that Smear infection into consideration. The pathogens can be transmitted primarily through the hands if there is insufficient hygiene and close contact.
The hand-mouth-foot disease is widespread among the population, so it has a high level of infection. This means that from a certain age almost everyone has come into contact with the disease. In most cases it is very harmless, if not completely without any symptoms. The most common group to experience hand, mouth and foot disease are young children under the age of 10. Of course, this disease can also occur in older children or adults, but mostly much less often than in small children.
Hand-Mouth-Foot Disease in Pregnancy
Usually it is enterovirus infection and hand, mouth and foot disease that develops from it harmless for the pregnant woman, as it usually has a mild course or runs completely without symptoms.
Because the enteroviruses in the environment Very common women are often confronted with them during pregnancy.
Especially during the Summer months and the following Autumn months the risk of infection is greatest.
Overall, there is unfortunately little information on whether an enterovirus infection during the pregnancy causes disease or developmental disorders of the fetus, or possibly even miscarriage.
What has been proven, however, is that a pregnant woman is infected with the enterovirus around the due date can lead to the fact that the pathogens can be transmitted to the newborn baby. In the vast majority of cases, too, there is a rather mild course.
In some cases, however, there may be a Infection of other organs like that Heart or also the liver come with potentially fatal consequences.
In the first two weeks of life of the newborn baby, the risk of a serious and complicated course of the disease is greatest with an infection with the enterovirus.








.jpg)





.jpg)