Colon inflammation
introduction
Of the Intestines, divided into Thin- and Large intestine, with its functions of mixing food, transporting food, splitting and absorbing food components and regulating the fluid balance, plays an essential role in the Digestive system a. The large intestine particularly takes on the task of Thickening (by dehydration) and Storage of the intestinal contents as well as its Onward transport up to excretion.

However, if an inflammatory disease occurs in this area, the sensitive system is disturbed. Colon inflammation does not initially mean that it is a disease of the colon as a whole functional system, but rather an isolated inflammation and damage to the colon mucosa.
In some cases, however, it is possible that the inflammatory process can spread beyond the mucosal barrier into the muscles of the large intestine. Colon inflammations are divided into three large groups "acute“, “chronic" and "ischemic“.
You might also be interested in this topic: Leaky Gut Syndrome
causes
The acute colon inflammation is one of the most common forms of Intestinal inflammation (2007 approx. 400,000 cases in Germany) and occurs in most cases combined with a Inflammation of the small intestine (Enterocolitis) and or Stomach (gastroenteritis) on. You will usually go through Viruses, bacteria (Salmonella, Shigella, Campylobacter, Escherichia coli, Clostridia, Staphylococci), Mushrooms or Parasites/ Protozoa (Amoeba) triggered that usually fecal-oral so it can be transferred by the inclusion of contaminated drinking water, infected food or through Contact with excretory products from sick people comes to infection. But also Medication intake (Antibiotics induced pseudomembranous colitis) and Radiation of abdominal tumors can cause acute colon inflammation.
To the chronic colon inflammation (CED; inflammatory bowel disease) count primarily the Crohn's disease and the Ulcerative colitis. The latter is an intermittent inflammation exclusively of the colon mucosa, which is usually in the last section of the Rectum begins and rises extensively, without interruptions and can affect other sections of the colon. The inflammation remains, however strictly limited to the colon, of the Small intestine is not affected. In 50% of cases, both the rectum and the sigmoid (Colon) affects the entire large intestine in 25%.
It is different with that Crohn's diseasewho also has one batch-wise course shows, but on the one hand shows inflammation beyond the mucous membrane (up to the large intestine muscles) and on the other hand not only shows the large intestine, but all structures of the digestive tract from the mouth to the anus can attack. The spread of inflammation is there not continuously as in ulcerative colitis, but rather discontinuously, so that there is a juxtaposition of healthy and diseased, inflamed intestinal sections. These are the most common Ileum (Ileum) and the Large intestine. The number of new cases for both forms of the disease is approx. 5 / 100,000 inhabitants / year and the frequency peak of the first manifestation is identical - it is between the ages of 20 and 40.
The root cause has not been conclusively clarified either for ulcerative colitis or for Crohn's disease. However, one is suspected Disorder in the immune system (Autoimmune reaction) leading to dysregulation of the the body's defenses and there is an uncontrolled, permanent inflammatory reaction with subsequent destruction of the mucous membrane. Of the Main risk factor for developing Crohn's disease that is Smoke (2-fold increased risk), but in ulcerative colitis it has a more protective effect (smokers are less likely to get sick). In both chronic inflammatory colon diseases there is often one family history.
The so-called "ischemic" colon inflammation is a non-infectious disease that arises from circulatory disorders in the colon. The reason for this is usually an increasing calcification of the intestinal vessels (in generalized arteriosclerosis), which leads to constrictions or occlusions and causes a reduced blood flow in the intestinal sections supplied by them.
diagnosis
Due to the mostly harmless, short and self-limiting course of acute colon inflammation, diagnosis beyond the anamnesis and physical examination is usually not necessary. If the symptoms are very severe, stool and blood tests for pathogens can be carried out.
The method of choice for diagnosing Crohn's disease is the mirroring of the large intestine and ileum with simultaneous tissue sampling, which is examined microscopically. Additional diagnostic measures can include an extended examination of the esophagus, stomach, and small intestine, and an x-ray or ultrasound examination of the abdomen. Blood tests in Crohn's disease patients show increased inflammation and anemia due to iron and / or folic acid deficiency. The same applies to the diagnosis of ulcerative colitis.
Read more on the topic: Ultrasound of the abdomen
Ischemic colitis is by default caused by a Colonoscopy (Colonoscopy), but an X-ray image of the abdomen and an X-ray image of the large intestine and / or the intestinal vessels using contrast media can also be used here.
Symptoms

Characteristic for acute colon inflammation is the sudden onset and short course from approx. 2-4 days, whereby the infection is self-limiting. The affected person usually suffers from severe diarrhea, whereby these are usually thin to watery. In more severe cases you can too mucus-, blood- or Pus admixture stand out in the chair. Can accompany fever, nausea and Vomit such as cramping abdominal pain occur.
The common symptoms of inflammatory bowel disease are also Diarrhea, nausea, Loss of appetite, fever and Weight loss. Another characteristic feature is the slow and creeping beginning and a in bursts (alternating symptom-free and symptom-rich intervals) progression of the disease. However, periods of constipation or normal stool can occur very rarely. This fact does not rule out colon inflammation.
The Crohn's disease- 90% of patients suffer from right-sided or abdominal pain near the belly button, fever, Flatulence and mostly bloodless diarrhea. 30% of those affected also have one Lactose intolerance (Lactose intolerance).
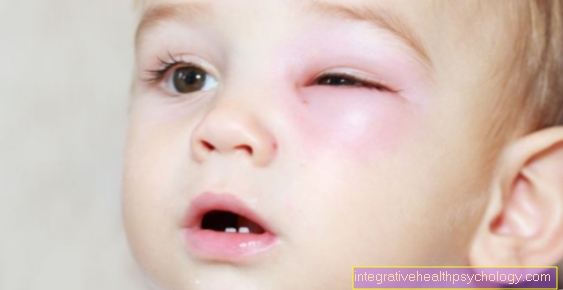
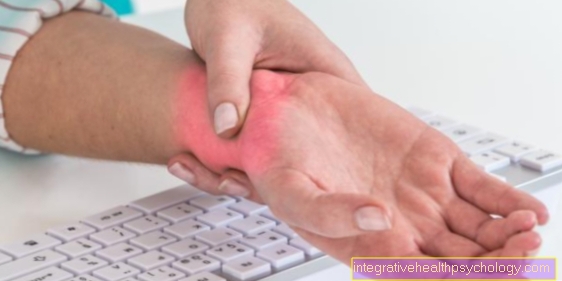
In contrast, the Ulcerative colitis bloody slimy diarrhea (up to 20 per day) caused by cramping abdominal pain to be accompanied. Side effects like Reddening of the skin, Joint pain and Inflammation of the eyes can rarely accompany ulcerative colitis, but significantly more often accompany Crohn's disease.
The ischemic colon inflammation Is characterized by intermittent abdominal pain and bloody or bloodless Diarrhea out. A complete occlusion of the large intestinal vessels can lead to a Bowel infarction (Mesenteric infarction) come to a Die of the affected part of the intestine and life threatening can be. Frequently, the affected patients also show calcifications in other areas of the body, for example too Circulatory disorders in the legs or the Coronary arteries being able to lead.
The main danger with all forms of inflammation lies in this high fluid and electrolyte losscaused by the diarrhea. Due to the inflammation of the mucous membrane, the large intestine is no longer able to absorb salts and water, so these are lost. The result can be a lack of fluids in the body, which is called Dehydration referred to as. Those affected can go through Weight loss and significant limitation in their physical performance stand out.
In chronic colon inflammation, another complication is above all Rupture of the intestinal wallwhich results from an increasing inflammatory destruction of the intestinal wall. Follow like Bleeding and a Spread of inflammation to the entire abdomen up to Blood poisoning are possible.
It can also cause inflammation too Adhesions of the intestine which can lead to a flow disruption with feces accumulation.
People with Crohn's disease, but even more so with ulcerative colitis, have an increased risk of developing one over the course of their life, depending on the duration and severity of the illness malignant colon tumor to get sick (colorectal cancer). Approx. 2% of ulcerative colitis patients develop colon carcinoma after a 10-year course of the disease, and after 30 years already about 30%. Another complication specific to ulcerative colitis is the development of a acute enlargement of the colon (toxic megacolon) in one shock and Multiple organ failure can end.
therapy
The treatment of light, self-limiting, acute colon inflammation consists of only one adequate fluid and electrolyte supply (salty liquids, fruit, carbohydrates, drinking water) and possibly the administration of Medication for diarrhea (Antidiarrheal: Loperamide). In severe cases with signs of dehydration, a Hospitalization with the administration of liquid (glucose-salt solution) via a drip and possibly a Administration of antibiotics (Fluoroquinolones: Ciprofloxacin) at bacterial infections become necessary.
The Therapy of Crohn's disease consists of two different components: one is one medical therapy initiated, initially Corticosteroids (rectally as a suppository or orally as a tablet), with increasing severity also Immunosuppressants (e.g. Azathioprine) and or Biologicals (TNF? Blockers: e.g. Imfliximab) can be used. On the other hand, general measures can be taken that support drug therapy, including z. B. the Stop smoking, one diet and the replacement of substances lost in the intestine in case of deficiency symptoms (iron, fat soluble Vitamins etc.) belong.
The same applies to the supportive Therapy of ulcerative colitisHowever, the drug therapy differs somewhat here: in the case of light to moderate attacks, it is initially used locally (rectally as a suppository) or systemically (orally as a tablet or granulate), which is more effective 5-aminosalicylic acid (Mesalazine). Additional use of is only made in the event of severe attacks Corticosteroids, Immunosuppressants and Biologicals.
A surgical intervention is only required in both acute and chronic colon inflammation if Intestinal wall perforations, Bleeding or Tumor development exist.
In the ischemic colon inflammation should be one in the acute stage oral food intake should be avoided, possibly can also take Blood thinners be useful (e.g. ASS). Narrowed or completely closed intestinal vessels should be made passable again as soon as possible, either by means of a drug or surgical intervention can be done. Already dead intestinal sections must be surgically removed.
Medication
If there is an acute colon inflammation, it is often a gastrointestinal infection with diarrhea and possibly vomiting. The rule here is that you should ensure that you drink enough fluids. Food intake should be avoided in the acute phase. Usually the disease is self-limiting and disappears after a few days. Medicines such as loperamide can be used for agonizing diarrhea. Loperamide inhibits bowel activity and thus alleviates diarrhea.
In the presence of chronic inflammatory bowel disease, drug therapy is extremely important. Cortisone preparations, immunosuppressants such as azathioprine and ciclospoprine A, aminosalicylates such as mesalazine and so-called biologicals such as infliximab or adalimumb are used here. Cortisone preparations are often used in acute attacks. Biologicals are relatively new drugs that are used when the others mentioned do not have a sufficient effect. They must be given regularly, usually by injection, and are very expensive.
homeopathy
If there is a chronic inflammatory bowel disease, it should be treated urgently by a doctor. If left untreated, the disease often progresses faster than with adequate drug therapy. To the homeopathic remedies, that are used to treat chronic colitis include, among others Schüssler salts. The various salts are said to have effects such as anti-inflammatory effects, a reduction in loss of appetite and a reduction in symptoms of weakness.
Other homeopathic remedies are for example Arsenicum album and Phosphorus. These should help against diarrhea and abdominal pain. It should be emphasized once again that medical treatment is essential for chronic inflammatory bowel disease, homeopathic therapy alone is not sufficient. In the case of acute inflammation of the intestine in the sense of gastroenteritis, active substances such as Plumbum metallicum and Sodium sulfuricum be helpful. These are said to provide relief from abdominal pain and diarrhea.
nutrition
In the presence of an acute gastrointestinal infection (gastroenteritis) should no food intake respectively. However, you should drink a lot to make up for the fluid deficit caused by the diarrhea. After the acute phase, there should be a slow diet with a light diet. Spicy and fatty foods should be avoided. In the group of inflammatory bowel diseases, it is important in an acute episode to supply the body with sufficient calories, but not to stress it. White bread, vegetable broth or a light potato soup, pureed fruit, oat flakes and easily digestible meat and fish dishes come into question here.
forecast
The acute colon inflammation usually have an sRapidly fading and self-ending, complication-free course.
Crohn's disease patient have high Recurrence rate (frequently recurring symptoms after symptom-free phases) and a 70% probability of having to undergo an operation within 15 years due to complications. A definitive cure through surgery is not possible in Crohn's disease.
However, it is different with the Ulcerative colitisthat through a Surgical removal of the entire colon definitely cured can be.With long-term and widespread illness, the risk of colon cancer increases significantly.
The prognosis of a ischemic colon inflammation depends crucially on early detection and initiation of therapy. In the early stages of this life-threatening disease, there is still a 95% chance of survival. B. 24 hours until the intervention, this drops to below 15%.






.jpg)