Joint effusion
definition
Joint effusion is the pathological accumulation of fluid within a joint. Depending on the type of fluid, a distinction is made between different types of joint effusion:
If the fluid is bloody, it is called hemarthrosis, if it is purulent, it is called this Pyarthrosis or Joint empyema. If only the amount of regular synovial fluid (Synovia) is increased, but the composition is as always, so is one Hydarthrosis in front.
causes
There are various causes that can trigger joint effusion.
The most common are trauma (then often as a bloody joint effusion) and inflammation of the inner synovium (often with pus). Degenerative diseases such as osteoarthritis or permanently existing incorrect loads can also lead to joint effusion.
In addition, there are some diseases that can be associated with joint effusion in some cases and that should definitely be clarified in order to be able to treat them adequately. These include tumor diseases, rheumatoid arthritis, gout and blood clotting disorders such as hemophilia.
Symptoms
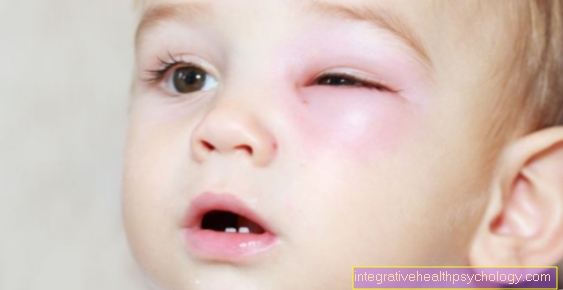
The main symptoms of a joint effusion are swelling, which is usually both visible and palpable, and pain in the affected joint. These exist mainly during exercise and exertion, but are usually noticeable at rest. The above complaints often lead to limited mobility of the fluid-filled joint.
If the joint effusion is caused by inflammation, there are often two other classic signs of inflammation, namely overheating and reddening.
Appointment with ?

I would be happy to advise you!
Who am I?
My name is dr. Nicolas Gumpert. I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
In order to be able to treat successfully in orthopedics, a thorough examination, diagnosis and a medical history are required.
In our very economic world in particular, there is too little time to thoroughly grasp the complex diseases of orthopedics and thus initiate targeted treatment.
I don't want to join the ranks of "quick knife pullers".
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You will find me:
- Lumedis - orthopedic surgeons
Kaiserstrasse 14
60311 Frankfurt am Main
You can make an appointment here.
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
For more information about myself, see Lumedis - Orthopedists.
diagnosis
To make the diagnosis of joint effusion, it is first of all of great importance to take a detailed medical history (anamnese), as this can be very indicative of a possible cause.
In addition, the joint should be thoroughly examined by the doctor.
In addition, there is usually a puncture from the joint effusion (Arthrocentesis).
This has two advantages:
On the one hand, you can send the liquid to the laboratory and have the puncture examined there (for example for bacteria or blood), on the other hand, it also means treating the patient by relieving the pressure on the joint.
If the cause of the effusion is still unclear, imaging (ultrasound, magnetic resonance tomography, computed tomography, x-ray) or arthroscopy (arthroscopy) can be used as a supplementary diagnostic procedure.
Read more about this at: Knee puncture
therapy

The treatment of joint effusion depends on the cause of the joint effusion and its underlying disease.
First of all, of course, one tries to create relief through conservative therapy.
Conservative therapy
At the beginning there should definitely be a relief of the joint and, if necessary, a splint of the affected area.
If possible, muscle exercises can lead to better drainage of the effusion.
In addition, you can achieve further pain relief with painkillers. The pain relievers can either be taken orally or injected.
The class of painkillers that is often used here and that has an anti-inflammatory effect is called nonsteroidal anti-inflammatory drugs, NSAIDs. The non-steroidal anti-inflammatory drugs also include ibuprofen and diclofenac.
Then there is the use of antibiotics.
Another conservative measure is to use compresses to cool the affected area, which can relieve the inflammation and pain. Elevating the affected area can also be helpful in order to better absorb the effusion.
The effusion may disappear by itself through conservative measures through resorption, but the unexplained cause of the effusion remains, which can lead to a recurrence of effusions.
Acute therapy
Acute therapy is a puncture of the joint.
This can be useful, especially in the case of unexplained causes of the effusion, in order to better diagnose the cause.
However, one should not forget that in most cases relieving the knee joint is not the solution to the problem, as the cause of the disease persists and the effusion is often only a side effect of another disease.
After the puncture, an elastic wrap is made with a felt ring.
Relief through puncture usually provides rapid pain relief by relieving pressure on the joint.
In addition, a medication can be injected into the joint at the same time if necessary. During the puncture with the hollow needle, value should be placed on high sterility standards, as otherwise an infection triggered by the puncture can occur.
The puncture is usually done after a local anesthetic of the area.
Operative therapy
If the suspicion of an infection of the knee joint is confirmed, surgical treatment should be initiated immediately.
Because an infection of the knee joint is an emergency situation, in which one should act surgically and initiate broad antibiotic treatment.
Otherwise, the specific cause can be searched further. During the operation you can repair fractures, cruciate ligament tears or remove part of the synovium.
The appropriate therapy for a joint effusion therefore depends on its cause. Relief with the help of a puncture is recommended in any case, as well as initially cooling, protection and immobilization of the affected joint (possibly elevated position), then later gradual mobilization.
Non-steroidal anti-inflammatory drugs are recommended for pain relief.
Whether further drug treatment or even an operation is necessary depends on what triggered the effusion.
If there is an underlying disease, it should of course also be treated.
In summary, it is important to ensure rapid treatment, as long-term joint effusions can lead to further consequential damage such as damage to the joint cartilage.
Puncture the joint effusion
If a patient is suffering from a joint effusion, in some cases it makes sense to puncture the effusion. The effusion is punctured with a thin needle under sterile conditions in order to remove fluid via a syringe or to inject medication.
Puncturing makes sense in three ways. When asked about the exact cause and extent of the joint effusion, it can be punctured for diagnosis.
A few milliliters of fluid are withdrawn so that you can quickly see whether there is blood or pus. Furthermore, this sample can be examined microbiologically and possibly a pathogen identified. On the other hand, you can puncture a joint effusion with therapeutic intent.
In many cases, the fluid in the joint exerts a painful pressure and cannot be absorbed by the body, so that here the joint effusion is removed from the joint space by puncturing to relieve the pressure.
Puncturing will help contain the inflammation, especially if pus is a major part of the fluid. In addition, doctors puncture a joint effusion to apply medication directly to the affected area. This is often done with cortisone.
However, the indication to puncture a joint effusion should always be narrowed down because the puncture itself can penetrate external pathogens and cause inflammation.
Therefore, special attention must be paid to sterility and care.
You can find much more information at: Knee puncture
forecast
If the joint effusion had a simple cause, such as a one-time trauma, it will usually go away after the joint puncture and will not return.
In some cases, however, several punctures have to be made. Then the person affected is symptom-free again.
In patients with an underlying disease, the prognosis of joint effusion depends primarily on the right therapy for the underlying disease.
If, for example, hemophilia (hemophilia), psoriatic arthritis (inflammation of the joint caused by psoriasis) or osteoarthritis remain undetected, the patient may initially be completely symptom-free again after the effusion has been relieved, but it is very likely that it will again be in the course of the disease joint effusion and possibly other problems.
Therefore: The cause of the effusion in the joint must always be identified in order to prevent further occurrence.
Joint effusion in the shoulder

causes
Joint effusions of the shoulder are usually caused by inflammation of the shoulder joint.
Degenerative changes / injuries
Especially in older people, degenerative changes can be the cause of shoulder inflammation.
These are caused by wear and tear. Here, for example, the attachments of the tendons can become calcified or the tendons can be torn or frayed.
If the irritation is too strong, the tendon can become inflamed.
But even minor accidents can cause major shoulder damage in older people with a previously damaged shoulder joint. For example, bone fractures or tearing of the muscle tendons can also trigger inflammation.
Bursitis can also trigger shoulder joint inflammation.
Septic inflammation of the shoulder joint
An inflammation of the shoulder joint can occur, for example, in a septic inflammation, where the inflammation had a different origin in the body and was carried over to the shoulder region.
The pathogens of the infection can settle again if they are spread via the blood and trigger inflammation.
Most often this happens with a protracted pneumonia and a weakened, suppressed immune system.
A particularly weakened immune system is found in cancer patients, elderly patients, pregnant women, or in patients with immune diseases.
Side effects of septic inflammation are pain in the shoulder region, redness, swelling, fever, malaise and the effusion.
Rheumatic inflammation in the shoulder joint
The presence of an underlying rheumatic disease can also cause shoulder joint inflammation and thus also an effusion.
Involvement of the shoulder joint as a concomitant disease occurs in 50-90% of rheumatism patients.
The patients usually have recurring swellings, effusions and pain in the shoulder joint.
Diagnosis
First of all, typical signs of inflammation can often be seen in the presence of an effusion, such as overheating, swelling and redness.
The patient would not tolerate this for long when palpating, because he would probably express too much pain, and there is also a severe restriction of movement.
Because of the severe restriction of movement, shoulder joint inflammation is also known as "frozen shoulder“Or shoulder joint stiffness.
Therefore, it is preferable to diagnose with the help of devices.
An ultrasound machine can usually make an effusion clearly visible. If you are unsure of the underlying disease or want to determine the exact cause, you can then puncture the effusion under ultrasound control.
The puncture is done with a fine hollow needle. The liquid can then be tested for pathogens such as bacteria or viruses, rheumatoid factors, cells, etc.
You can also have an X-ray taken to assess the extent of the shoulder joint damage. An MRI scan is sometimes necessary.
therapy
Treatment consists of treating the underlying disease.
In the case of septic inflammation, this means, on the one hand, fighting the root cause of the delayed disease in order to get the inflammation out of the shoulder. This is done with a surgical procedure and thus cleaning and rinsing the joint. Antibiotic therapy should also be initiated.
In the case of an underlying rheumatic disease, there are special anti-inflammatory drugs that can be used and the use of cortisone.
Depending on the extent to which the joint is affected by the rheumatic disease, surgical rehabilitation up to and including an artificial joint replacement may be necessary.
Conservative therapy
Painkillers and anti-inflammatory drugs can be used conservatively. These include the pain reliever class of non-steroidal anti-inflammatory drugs such as ibuprofen, diclofenac or ASA. The drugs can be used orally or by injection into the shoulder joint.
Operative therapy
The surgical treatment is always carried out using the keyhole technique in the form of a joint reflection (Arthroscopy).
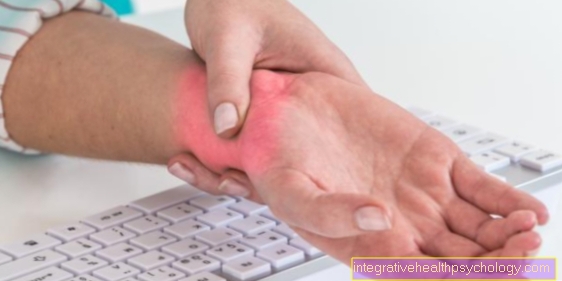
Joint effusion finger / thumb
An effusion on one or more fingers can have different causes.
On the one hand, there are inflammatory diseases that can contribute to swelling. Joint inflammation is also called arthritis, and it can have various causes itself.
Joint inflammation / arthritis
The most common cause of arthritis is rheumatoid arthritis, whereby the fingers are very often affected with both hands.
The joint effusion is usually accompanied by other signs of inflammation such as overheating, reddening, pain and functional restrictions.
After rest breaks there is usually a feeling of stiffness, which gradually disappears again through movement.
In the course of this, rheumatoid nodules can also form on the fingers.
However, there are other causes of joint inflammation as well. Because an infection with pathogens such as bacteria or viruses can also trigger joint inflammation.
There are also various metabolic diseases, such as gout, which can trigger joint inflammation, or autoimmune diseases.
Autoimmune diseases with frequent joint inflammation include: rheumatoid polyarthritis (Rheumatism with inflammation of the joints in several joints), Psoriasis (a rheumatic disease with an additional attack on the skin as psoriasis) and Bechterew's disease (also a rheumatic disease, where the spine is particularly badly affected) or scleroderma (the skin is also affected here).
Joint wear
Wear and tear on the joints (osteoarthritis) on the fingers can also lead to joint effusion and inflammation. The wear and tear of the joints causes irritation due to friction, which can trigger inflammatory reactions such as joint effusion.
trauma
Joint effusion in the fingers can also result from trauma.
In addition to fractures and bruises, so-called capsule ruptures often occur in the fingers. The capsule usually provides the necessary stabilization for the fingers and is often damaged in handball sports, such as volleyball, handball, basketball or martial arts.
A jerky blow can cause the capsule to overstretch or tear.
If the capsule ruptures, it is recommended to first cool the area so that the finger swells a little again.
Painkillers can also be given. The capsule rupture can usually be recognized by the functional impairment of the fingers with swelling and throbbing pain.
The doctor usually recognizes this immediately by palpation and slight movement. In addition, an X-ray is usually taken to rule out possible breaks.
As a treatment, a bandage is put on here, which is worn for about two weeks.
Joint effusion hip
The hip is the most stressed joint in the body due to its size.
Therefore, joint effusion can also occur here.
In this case it is difficult to walk and mobility in the hips is limited. The joint effusion is not as visible on the outside of the hip as it is on the knee or ankle, but it also causes pain, especially when moving.
These can radiate into the lumbar spine.
causes
The main causes of joint effusion in the knee are degenerative, i.e. wear-related and inflammatory diseases. Above all, activated coxarthrosis is responsible for joint effusion.
This is wear and tear on the joint surfaces in the hip. The disease mainly occurs in old age. The joint effusion comes about here due to the inflammation of the synovial membrane, through which more joint fluid is formed.
Other typical causes are trauma and overloading of the joint, especially in the context of sport. Children and adolescents often suffer from coxitis fugax, an inflammation of the hip with joint effusion.
diagnosis
First, the general mobility of the hip is checked and the hip is palpated. In addition to the restricted mobility, there is usually pain on pressure over the hip joint. In the case of joint effusion in the hip, equipment measures are then used to detect the joint effusion.
At the beginning there is the ultrasound, which can non-invasively visualize the joint space by an experienced examiner and estimate the amount of fluid in the joint. If this examination is not sufficient, an X-ray examination or an MRI may be appropriate.
In addition, in some cases a diagnostic puncture is indicated for joint effusion.
In addition to relieving the pressure on the joint, this can be used to determine whether it is serous fluid, pus or blood.
therapy
At the beginning there is the attempt to treat the joint effusion in the hip conservatively. Elevation, cooling and protection are the most effective measures here.
Non-steroidal anti-inflammatory drugs such as diclofenac or ibuprofen can be given as support. If bacteria are detected, antibiotics are indicated.
Another option is to inject cortisone directly into the joint. Cortisone has an anti-inflammatory and decongestant effect, but this measure is controversial because of the risk of infection. Surgical therapies are the last resort for joint effusion of the hip, but are essential if structures are damaged.
Joint effusion in the knee
Joint effusion in the knee is not uncommon.
There are various possible causes that can cause joint effusion in the form of synovial fluid or blood in the event of traumatic events and pus in the case of infections in the knee.
A distinction should be made between acute and chronic joint effusion.
It is noticeable through a swollen knee that is associated with pain and restricted movement.
causes
Typical causes of acute joint effusion in the knee are injuries of all kinds.
In the foreground are injuries to joint structures caused by accidents.
An injury to the ligaments such as the cruciate ligament almost always leads to an effusion, but damage to the menisci also causes fluid to accumulate in the knee.
Popping out the kneecap makes the knee swell just as often.
In addition, a joint effusion in the knee can be a sign of excessive exercise through exercise without damaging a structure. Especially in older people, wear-related processes in the context of osteoarthritis are in the foreground, which are often associated with joint effusion in the knee.
Another group of diseases that can cause an effusion in the knee are rheumatological diseases. Although the knee joint is usually not the main affected site of manifestation, it must be remembered.
A chronic joint effusion in the knee is a typical sign of a bacterial infection. In this knee joint inflammation, the germs either enter the joint from the outside through invasive interventions or injections or, in the case of general infections, reach the knee via the blood.
diagnosis
In addition to the anamnesis, the beginning of the diagnosis of joint effusion in the knee is the physical examination.
A swollen knee and pain are the first clues.
The best known clinical sign is the "dancing patella". With both hands, the knee is stroked towards the patella, whereupon the patella offers elastic resistance to frontal pressure.
The kneecap floats on the effusion.
Reddening and overheating of the skin indicate infectious events.
You can safely recognize the effusion by means of:
- Ultrasonic
- CT
or - MRI of the knee
Surely the simplest method is certainly an examination. A knee joint effusion above a certain size can be safely felt by an experienced examiner.
therapy
The therapy depends on the cause of the symptoms. A simple joint effusion in the knee can be treated with immobilization, cooling, and oral anti-inflammatory drugs such as diclofenac.
If there are significant symptoms such as a purulent effusion, a knee puncture may be necessary to relieve the joint. This must be done under absolute sterility. At the same time, cortisone can be applied directly to the site of action during the puncture.
Structural damage such as a meniscus or ligament tear usually requires surgical treatment.
You can find much more information under our topic: Joint effusion in the knee
Joint effusion ankle
Due to the everyday stress on the ankle, joint effusion is not uncommon at this point.
With pain, swelling and loss of function, the symptoms are typical symptoms of joint effusion.
causes
Joint effusion also has various causes on the ankle, above all traumatic events. Typical is the twisting, technically called supination trauma (twisting outwards).
It is the most common sports injury ever. The joint effusion in the ankle occurs because the lateral ligaments on the ankle are overstretched and the capsular apparatus of the joint is also heavily strained.
A subsequent inflammatory reaction in the body leads to swelling and pain. Ligaments and blood vessels can also tear, which worsens the joint effusion in the ankle and is usually supplemented by a pronounced bruise. Broken bones on the ankle also cause joint effusion. In addition to the traumatic events, degenerative and infectious processes also cause joint effusion. Osteoarthritis, i.e. the loss of articular cartilage and bone substance caused by wear and tear, is particularly important in old age.
Arthritis is also not uncommon, i.e. inflammation in the ankle.
It can be caused by pathogens such as bacteria or non-infectious in the context of rheumatological diseases or gout.
In all cases there is a joint effusion on the ankle, which can be more or less pronounced.
diagnosis
At the beginning, in addition to taking the medical history, the doctor will clinically examine the ankle. The swelling, along with pain and possibly reddening, quickly indicates that there is a joint effusion.
The mobility in the joint can be evaluated with a few tests. In order to determine the cause and the extent more precisely, examinations such as ultrasound and X-rays follow.
Bony involvement can hereby be confirmed or excluded. If an infectious joint effusion is suspected on the ankle, the effusion can be punctured to detect pus or blood.
In rare cases, tests for rheumatoid diseases complement the diagnosis.
therapy
The therapy for joint effusion on the ankle depends on the type of symptoms. Injuries are initially treated conservatively with rest, cold and also anti-inflammatory drugs. Depending on the type of fracture, fractures can result in surgery. Antibiotics are indicated for pathogen-related joint effusion. A puncture of the ankle can also be considered to relieve the effusion.








.jpg)