Ulcerative colitis flare-up
definition
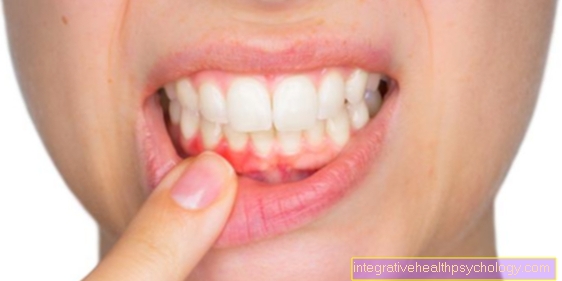
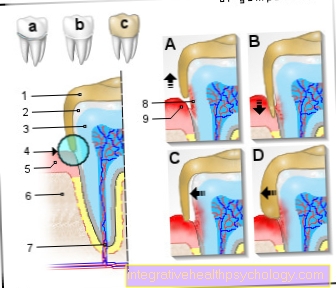
The course of ulcerative colitis alternates between phases of acute inflammation of the intestinal mucosa and phases of remission in which no inflammatory activity is detectable and, as a rule, no symptoms occur. The phases of inflammation of the lining of the intestines are known as flares. The inflammation damages the mucous membrane in the intestine and the typical bloody diarrhea occurs.

causes
The exact causes that can trigger a flare-up of ulcerative colitis are not exactly known. Even the causes for the occurrence of the disease are largely not yet understood. Stress or emotionally stressful situations are brought into the context of being able to trigger a surge. The causes of a flare-up cannot be precisely determined and vary from patient to patient.
Read more about this at: Causes of ulcerative colitis
From a cold
In the medical literature there is no clear connection between a cold and an acute flare-up. Nevertheless, it is not inconceivable that a cold can be the trigger for a flare-up in an individual patient.
How can you spot a surge?
A relapse can be recognized by the sudden appearance of the typical ulcerative colitis symptoms (see accompanying symptoms).
The markers CRP (C-reactive protein) and BSG (Sedimentation rate) be increased. They are classic markers of inflammation and can be used to monitor the course of the inflammation. In addition, excessive bleeding from the rectum or bloody diarrhea can lead to anemia, which can also be detected in the blood count.
Read more about this under
- CRP value
- Inflammation in the blood
In the examination of the stool, two markers that speak for the mucosal inflammation can also be detected. These are calprotectin and lactoferrin. In addition, a bacterial cause for the acute onset of diarrhea can be excluded in the stool.
Sonography can be used as an imaging option to detect a surge. During an acute episode, sonography can detect a thickening of the wall layers of the colon. Normally, despite the thickening, all wall layers of the large intestine can still be neatly separated from one another. Further diagnostics are usually not necessary and would only be carried out if the patient has not yet been diagnosed with a chronic inflammatory bowel disease such as ulcerative colitis.
Concomitant symptoms
The main symptom of a flare-up is bloody diarrhea in variable amounts. These can occur daily in variable amounts. If the episode is severe, there are more than six bloody diarrhea a day. As you can see from this example, the severity of the individual flare-up can also be assessed from the severity of the accompanying symptoms.The diarrhea can also be associated with pain during bowel movements or abdominal pain. These are often located in the left lower abdomen.
As a lot of water is excreted from the body in a short time due to the diarrhea, weight loss and dehydration regularly occur. Dehydration means that the body's water content is too low. Since the blood loss can be significant depending on the frequency of bowel movements and the strength of the bleeding, weakness due to anemia is also an accompanying symptom. In extreme cases, blood loss can be so great that shock can occur. Shock is described in medical terminology as a condition in which not enough oxygen can be transported to organs and other tissues. This condition can be triggered, among other things, by high blood loss.
Read more about this under Symptoms of shock Fever is also a typical symptom of a flare-up, especially a severe flare-up. With a slight flare-up, a fever may not appear as a symptom. Patients continue to report feeling sick. In severe attacks, an increased pulse rate of over 100 beats per minute is found in the patient.
Read more about this under Symptoms of Ulcerative Colitis
Without diarrhea
An acute flare-up without diarrhea is rather untypical for ulcerative colitis because it is the main symptom of a flare-up. The frequency of the diarrhea is therefore also an important parameter in order to be able to assess whether it is a slight or a severe flare-up. If fever and an increased feeling of illness are given as symptoms, without diarrhea, other causes for the symptoms described should also be investigated. Crohn's disease, which is also an inflammatory bowel disease, is more likely to run without diarrhea.
Read more about this under Symptoms of Crohn's Disease
fever
Fever can be a symptom of an acute flare-up of ulcerative colitis. With a slight thrust, temperatures of up to 37 degrees Celsius are to be expected, at which one cannot yet speak of fever. In moderate thrust, feverish temperatures of up to 38 degrees Celsius tend to occur. Even higher temperatures are classic in a severe episode, whereby the body temperature of the individual patients can of course vary and the values given are therefore only guidelines.
treatment
The therapy of the thrust is adapted to how strong the individual thrust is.
In the case of a slight episode with only a few bloody diarrhea and no fever, 5-ASA preparations, such as mesalazine, are used in acute therapy. These counteract the inflammation in the intestinal tract and trigger a slight immunosuppression.
A moderate episode is characterized by a distinct feeling of illness with regular bloody diarrhea and a slight increase in temperature. In addition to the 5-ASA preparations, glucocorticoids can only be given locally and in tablet form if there is no improvement.
In the severe episode, which is accompanied by severe feelings of illness, frequent bloody cases and fever, the therapy must be increased even further. First a therapy attempt with glucocorticoids (e.g. Prednisolone) started via the vein. It is hoped that the drug will have a better effect when administered through a venous access. If this does not improve, therapy with immunosuppressants can be considered. Common drugs are for example ciclospoprin A, tacrolimus or infliximab. However, since these immunosuppressants are not completely uncomplicated, surgical therapy should also be considered beforehand, as this can cure ulcerative colitis.
Read more about this under
- Therapy of ulcerative colitis
- Drugs for ulcerative colitis
Cortisone
Cortisone belongs to the group of drugs known as glucocorticoids. It is identical to cortisone, which is produced by the body itself. Cortisone is used in relapse therapy because of its anti-inflammatory and immunosuppressive effects. This should counteract the excessive inflammatory reaction of the body. However, since cortisone also has some relevant side effects, the drug must be used with caution and the dose must always be reduced in slow steps at the end of therapy. Some of these side effects are, for example, increased blood pressure, edema, breakdown of bone substance and the triggering of diabetes.
Read more about this under Side effects of cortisone
Duration
The duration of an attack varies with the severity of the attack and depends on the response to the acute medication. An episode can last anywhere from four to eight weeks. However, there are also forms of ulcerative colitis in which there is no inflammation-free interval. This process is called chronic-continuous. The intensity of the constant inflammation can vary greatly.
Read more on this topic at: Life expectancy in ulcerative colitis
Thrust in pregnancy
The probability of getting a flare-up during pregnancy is around 30%. The course of ulcerative colitis is not negatively affected by pregnancy. However, should a relapse occur, it must be treated as quickly as possible, as high inflammatory activity can have negative effects on the unborn child. The treatment is based on the graded scheme, which is also used for non-pregnant women. The medication should be given in sufficient doses because long-term inflammation can cause more damage than the side effects of the medication.
In the case of relapse therapy with cortisone in the last weeks of pregnancy, it must be noted that this can limit the cortisol formation of the fetus after birth. The newborns stand out with indifference and decreased activity. This deficiency can be treated well with temporary replacement therapy with cortisone. If it is a very severe episode that cannot be adequately treated with 5-ASA preparations and glucocorticoids alone, it is possible, after very strict assessment, to use the immunosuppressant Azathioprine to give. When taking it, however, both mother and child must be closely monitored. Other drugs to escalate therapy in severe relapses such as tacrolimus, ciclosporin A or the antibody infliximab should not be given during pregnancy.
Thrust while breastfeeding
In general, relapse therapy with 5-ASA preparations or glucocorticoids such as cortisone is possible during pregnancy. High-dose cortisone therapy during breastfeeding is also possible. However, it must be noted that cortisone is passed on to the newborn in breast milk. Similar to cortisone therapy during pregnancy, there may be a reduced formation of endogenous cortisol in the newborn. If the mother has to undergo cortisone therapy while she is breastfeeding, a pediatrician should check closely so that a deficiency can be quickly identified and treated.
If immunosuppressants such as methotrexate, azathioprine, tacrolimus or antibodies such as infliximab have to be used due to the severity of the attack, the newborn should no longer be breastfed because there is insufficient experience of how these drugs affect the newborn and in which case The extent to which they are transmitted through breast milk.