Eczema in the baby
introduction
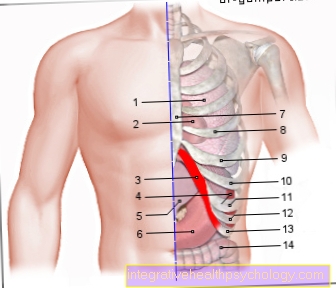
Eczema is a collective term for various skin diseases, the characteristics of which are reddening, swelling, blistering and oozing with the formation of crusts and scales on the affected skin area. Eczema is one of the most common skin diseases in babies. Typical localization of eczema in babies is the hairy head, face, especially cheeks and around the mouth (lat .: perioral), as well as the feet, hands and buttocks.
The triggers of eczema are numerous. So you can differentiate between different forms of eczema depending on the cause. These include, for example, toxic contact eczema, allergic contact eczema, atopic eczema (neurodermatitis in babies) or seborrheic eczema.

By definition, however, eczema in babies is not based on an infection, which is why eczema is a non-contagious skin disease.
The typical main symptom of eczema in babies, regardless of its trigger, is usually severe itching. Itchy eczema is also less common in babies. Since the intense itching can lead to constant scratching of the affected area of the skin and this can lead to injuries and, as a result, colonization with bacteria or viruses, eczema in babies should always be treated. Nourishing ointments, gels, lotions or baths are particularly suitable for this.
root cause
Eczema is caused by a disruption of the skin barrier, caused by external environmental factors or internal influences. The disruption of the skin's barrier function mediates an inflammatory reaction, which further maintains the skin's disrupted barrier function. The migration of inflammatory cells mediates the typical symptoms of eczema, such as reddening, swelling and blistering. Depending on the cause of this impaired skin barrier function, a distinction is made between different forms of eczema.
If the contact of the skin with toxic, aggressive substances (e.g. chemicals or strong radiation) leads to skin damage and a disruption of the skin barrier with reddening, swelling and blistering, this is referred to as toxic contact eczema.
A distinction is made between toxic contact eczema and allergic contact eczema, which is not triggered by toxic substances but by so-called allergens. These are various substances that trigger an excessive immune reaction in some people due to a hypersensitivity reaction to these substances when touched and thus ultimately cause a disruption of the skin barrier with the consequences mentioned. Substances that often act as allergens are nickel (nickel allergy), fragrances and flavorings, preservatives and latex (latex allergy).
Atopic eczema (Neurodermatitis) is also caused by a hypersensitivity reaction of the immune system to normally harmless substances, especially pollen, animal hair or house dust mites. Atopic eczema is often associated with other diseases such as hay fever or allergic asthma. Why these harmless substances such as pollen, animal hair or house dust mites lead to hypersensitivity reactions in some people has not been conclusively clarified. Since family members of the person concerned often suffer from atopic eczema, hay fever or allergic asthma, a genetic predisposition is suspected above all.
The three forms of eczema mentioned, toxic and allergic contact eczema, and atopic eczema form the main group of all eczema in babies. Another form of eczema that is also often found in babies is seborrheic eczema. The cause of seborrheic eczema has not been clearly established. A genetic predisposition, profuse sweating and moisture build-up in the skin due to wrong clothing or wrong skin care products are suspected.
Symptoms
The different forms of eczema in babies (such as toxic and allergic contact eczema, atopic eczema or seborrheic eczema) are based on different causes and mechanisms of disease development, but ultimately all result in a typical eczema reaction based on a disruption of the skin's barrier function .
This eczema reaction manifests itself in a blurred skin reddening with swelling and blistering. These blisters are filled with fluid and can be very itchy. Scratching or spontaneous bursting of the blisters causes the affected areas of skin to ooze. In most cases, the eczema heals with the formation of crusts or scales.
Typical localization of eczema in babies is the hairy head, face, especially cheeks and around the mouth (lat .: perioral), as well as the feet, hands and buttocks.
The above-mentioned forms of eczema can also become chronic. This means that eczema does not heal due to persistent irritation from the trigger, for example, but becomes chronic (long-lasting) become. Again, redness, swelling and blistering are the result. In addition, nodules can form. Eventually the skin will thicken, dry out, and flake, known as lichenification, which is typical of chronic eczema.
The main symptom of eczema in babies is usually pronounced itching, but there are seldom forms of eczema that do not itch. The massive itching can lead to constant scratching of the affected skin area, which can lead to small wounds. Problems arise when bacteria or viruses penetrate the scratched skin. The colonization of the wounded skin with bacteria or viruses is known as superinfection or secondary infection and significantly impairs the healing process of eczema in the baby.
Eczema on the baby's face
The first manifestation of atopic eczema (see also: Atopic dermatitis in babies) often begins in infancy of 3 months. Here, the eczema in the baby's face is usually one of the first localizations on the body. The reddened areas on the forehead and cheeks, which are later characterized by vesicles and nodules, are particularly evident. The entire lateral face and eyelids are further options for spreading. The eczematous complexion can spread to the whole face. Most of the time, severe itching occurs as a symptom of eczema, so that the child manipulates the affected areas. This usually causes insomnia at night and, due to the overtired state of mind, brings about unbearable behavior during the day. As a result of the manipulation, the skin can become inflamed and also begin to ooze. Atopic eczema can be summarized under the term neurodermatitis.
In addition to atopic eczema, it can also be infantile seborrheic eczema (inflammatory skin rash). This occurs as early as the first month of babies and manifests itself primarily in the face and head, on the cheeks, eyebrows, nose and forehead.
Read more on the subject at: Seborrheic eczema and atopic dermatitis
General information on the topic can be found here: Eczema on the face
Eczema on the baby's neck
A predisposed site of eczema in babies is the neck. As with the face, redness and nodular or vesicle-like skin changes occur. In most cases, these areas in the entire neck area are caused by neurodermatitis. The first visible skin changes usually appear in the area of the face or head and can spread over the neck to the trunk. The neck is rarely affected as a manifestation site in babies. When involved, the skin appears rather dry and lackluster due to an underactive sebum and sweat glands. It is advisable to control the baby's tendency to manipulate and to reduce its strength using gloves in order to avoid subsequent infectious diseases of the skin.
Eczema on the baby's head
The scalp as an environment rich in sebum and sweat glands is a part of the body in babies where eczema can often be observed. A characteristic phenomenon here is seborrheic eczema, which is represented by yellowish-greasy scales on a reddened scalp. The borders of the redness are sharply defined. The occurrence is frequent in infancy.
There are several possible reasons for eczema. It has not yet been clearly established whether the problem is increased sebum production, an infection of the hair follicles or hormonal factors. It should also be noted that atopic eczema (neurodermatitis) can be the reason for the onset of seborrheic eczema in around a third of cases. It is noticeable that there is usually no itching.
As a rule, the healing process sets in by itself and ends within a few weeks to months. A lot of fresh air and oil baths can provide support, as can glucocorticoid therapy (usually cortisone) and antimycotic therapy (therapy against fungal infections) in severe forms. Fungal infections can occur as a secondary disease due to reduced immune function in the area of eczema and delay healing.
Eczema on the cheeks
Redness around the cheeks can occur as a result of a baby's teething. Teething occurs at 6 months of age and can take up to three years of age for full dentition to form.
In the case of redness in the cheek area, care should be taken to see whether it is simply a result of teething. Here, reddening must be distinguished from eczema formation. Eczema on the cheeks usually has other causes. The atopic eczema of an infant should be considered, which can occur at this age without great risks. Itching, which is often observed, is characteristic here. Atopic eczema is summarized under the term neurodermatitis. However, few people who had severe eczema in infancy carry symptoms later. This means that in the majority of adults there are few or no symptoms. It should be noted that the cheeks are a predisposed point for neurodermatitis in early childhood.
Eczema when teething
Teething describes the breakthrough of teeth that have long been laid in the jawbone through the gums. This creates a pronounced negative stress in some babies, as the mechanical pressure or tension of the gums can often be accompanied by pain. It can be observed that at the point where a tooth erupts, redness can appear on the skin. These often show up in the cheek area. Irritation up to slight inflammation can be seen in the same place on the gums.
The reddening of the skin, exclusively as a result of teething, should not be regarded as eczema. When teething, more saliva is produced, which in babies is not only swallowed, but also escapes to the outside. Saliva already contains enzymes that initiate digestion and break down food components. With large amounts of saliva and certain dwell times on the skin, irritations can arise here, which lead to slight eczematous changes due to contact. Teething can even lead to an increase in body temperature, which should, however, be normalized again within 24 hours.
In the case of more serious defects of the oral mucosa, massive eczema in the cheek area, as well as continued increased body temperature (> 24h), a consequence of teething should be avoided. A pediatrician should narrow down the symptoms and, if necessary, initiate the indicated treatment.
Read more on the subject at: Teething in the baby
Eczema on the baby's arm
Most often, eczema in babies occurs on the extensor sides of the arm, such as the elbow. The arm can be seen as a further expansion area as a result of atopic eczema (neurodermatitis).Heralds are eczema on the head and face. The child often suffers from pronounced itching.
An attempt to alleviate the problem can be made by closely observing the child for any food or clothing that may trigger the child by avoiding certain foods or textiles. If the symptoms persist, medical advice should be sought.
Since eczema is predominantly an immune response, excessive immune responses can be treated locally on the skin. Usually, however, self-healing can be expected within a few weeks to months. With increasing age, there is usually a clear improvement, so that up to 70% of young patients have little or no symptoms during puberty.
Eczema on the baby's stomach
Redness on the abdomen can occur as part of atopic eczema. However, it is more likely that this is a contact allergy that occurs around 30% of the time. The triggering factors here are skin-irritating clothing, a cool and dry climate and metal alloys on items of clothing, for example in the form of a button.
In addition, lipid metabolism disorders can also cause skin changes that occur here. If you do not use substances that are causally irritating on the skin, there is usually an improvement. Overall, the degree of severity of a skin change in the context of a contact allergy is rather mild. In the case of acute deterioration, a contact allergy can be avoided. This could be a bacterial and / or viral secondary disease that can occur as a complication. Pediatrician advice should therefore be used.
Eczema on the baby's bottom
Contact eczema often occurs on the child's bottom or buttocks due to constant contact with incontinence pads / diapers and textiles, which can be referred to as diaper rash. Dermatitis is an eczematous inflammatory reaction of the middle layer of the skin. This results from the softening of the skin by urine and stool. In addition, the skin is confronted with the decomposition of urine with the formation of ammonia, in which an unusually high pH value also stresses the skin. This can lead to the activation of enzymes that dissolve the top layer of the skin.
Seborrheic eczema usually occurs in the genital area. It is therefore conceivable that due to the local proximity, an existing eczematous phenomenon in the area of the vagina and penis, as well as in the anal fold, can trigger skin irritations in the area of the buttocks. This can be remedied by regular skin cleaning and skin care in the skin-pH-neutral range, as well as preventing waterlogging by regularly ventilating the affected skin areas. This allows the skin barrier that is formed by the epidermis to regenerate again.
Eczema in the baby with itching
Eczema with itching occurs relatively often in infancy, usually in the context of neurodermatitis. The itching aggravates the actual eczematous change through additional damage to the organ. This is followed by a delayed healing process and a primarily resulting deteriorated skin condition. This means that a pronounced inflammatory reaction is provoked or further developed.
The psychological component of the child as well as the parents who suffer with their baby must be taken into account. The unbearable physical symptoms have a lasting effect on the daily routine and the day-night rhythm, so that an unbalanced mood can ensue on both sides. Thus, with persistent itching and irreducible symptoms by means of nursing measures, drug therapy is usually indicated. A relaxed psyche and lack of manipulation of the child accelerate the improvement of the symptoms. By foregoing treatment, psychological distress and the bacterial and mycotic infectious diseases that result from it can be provoked.
Eczema in the baby without itching
If there is no itching of eczema in the baby, it is usually the form of seborrheic eczema. This occurs mainly in areas with many glands, such as the T-zone on the face, the scalp, as well as in the neck and neck area. Since the itching turns out to be a complicating factor, a milder course of the eczema can be observed in some cases. As a rule, seborrheic eczema heals itself in small children and only requires supportive therapy. Examples of this would be exposure to the open air, careful compliance with hygienic measures to prevent further complications, and skin care with gentle care products. Topically (locally) the use of glucocorticoids may be an option if the course is complicated and lengthy.
diagnosis
Since the common appearance of redness, swelling, as well as oozing or crusted blisters is characteristic of eczema, eczema in the baby is a visual diagnosis. However, in order to determine the cause of eczema in the baby, a detailed survey of the parents (the so-called anamnese) required. The doctor asks whether the baby may have come into contact with toxic substances, which could indicate toxic contact eczema.
If the baby has been in contact with allergenic substances such as nickel, this could be an indication of the presence of allergic contact dermatitis.
The presence of other illnesses in the baby, such as allergic asthma or hay fever, can lead to suspicion of atopic eczema (Neurodermatitis) to steer. The occurrence of asthma, hay fever or neurodermatitis in the family would then further corroborate the suspected diagnosis.
The question of skin care products used in babies can also be useful, for example to diagnose seborrheic eczema.
In particular, to diagnose allergic contact eczema and atopic eczema, some test methods such as a blood test or a patch test, and less often a prick test, are also used. These test methods can be used to identify substances that cause hypersensitivity reactions in babies (so-called allergens).
therapy
Eczema is often accompanied by severe itching, which can lead to the affected skin areas being scratched open and small injuries occurring. Small injuries to the skin allow bacteria or viruses to colonize the skin. In order to avoid this so-called super or secondary infection with bacteria or viruses, eczema should always be treated.
First of all, various ointments come into consideration, which are applied to the affected areas of the skin, such as the hairy head, face, especially the cheeks, as well as feet, hands and buttocks. The consistency of the ointment depends on the stage of the eczema.
If the eczema occurs acutely and manifests itself primarily as redness, swelling and oozing, ointments with a high water content should be used. Is the eczema chronic (long-lasting), ointments with a high fat content should be used, as these protect the flaky, dry skin from further dehydration.
In the case of extremely itchy eczema, cooling gels, lotions or cold compresses can also be used as these help relieve the itching. Massive itching can also be treated with medication, with so-called antihistamines.
If the eczema becomes superinfected with bacteria or viruses, antibiotic and antiseptic ointments are also used. In worse cases, antibiotics must be given in the form of tablets.
However, the elimination of the cause of the eczema is of paramount importance. This means toxic or allergenic substances that have caused the eczema should be avoided in the future.
forecast
The prognosis for eczema in babies varies depending on the type of eczema. Toxic contact eczema, allergic contact eczema and seborrheic eczema have a good prognosis if the triggering substances are avoided and the skin is properly cared for.
The prognosis of atopic eczema (neurodermatitis), however, is difficult to predict. It depends, among other things, on the age of onset and additional diseases of the affected baby. The earlier atopic eczema occurs and the earlier the baby or child suffers from other diseases such as allergic asthma and hay fever, the worse the prognosis.
prophylaxis
Eczema often occurs on dry and sensitive areas of the skin. Therefore, among other things, by avoiding dry skin, good skin care can prevent the development of eczema in babies. Various measures can be considered for this. On the one hand, the skin should not be washed too often or too hot. To care for the skin, moisturizing lotions should be used that do not contain any fragrances or preservatives. In addition, care should be taken to ensure adequate hydration.
If the baby already has eczema and the trigger is known, further eczema can be prevented by avoiding the triggering substance.