Kidney Disease Diet
Synonyms in a broader sense
Renal insufficiency, renal failure
Chronic renal failure
A chronic renal failure (Function restriction) is characterized in that, as a result, urinary substances, in particular urea, uric acid and Creatinine increase in the blood serum and at the same time the amount of filtrate in the kidney gets smaller.
The disease process progresses more or less and a cure is no longer possible. The most important goal of therapy is to delay or stop the progression of the disease.

The most important tasks of the kidney include:
- Excretion of end products of metabolism, especially protein metabolism such as urea, Creatinine and uric acidwhich accumulate in the body when the kidneys are not functioning properly, causing uremia (Self-poisoning) can lead.
- Regulation of the water and salt balance such as sodium, potassium, calcium, phosphorus and the acid-base balance.
- Build-up and breakdown of hormones.
The healthy kidney produces about 1 - 1.5 l urine within 24 hours with which the waste products are excreted and their blood concentrations remain normal.
If a healthy person drinks large amounts of liquid, the amount of urine increases; if, on the other hand, he is thirsty, the kidneys secreted only a little, but highly concentrated, urine. The diseased kidney is no longer capable of this work of concentration. The kidney has an enormously high performance reserve and this fact is also evident from the fact that humans can normally survive with only one kidney. If the kidney falls ill, the remaining healthy tissue can take over the necessary tasks for a long time.
With chronic kidney disease, the kidneys initially only lose the ability to produce concentrated urine. Sufficient water must therefore be available for the waste products to be eliminated and 2-3l must be drunk daily.
With this ample amount of drinking, the kidneys can continue to excrete the urinary substances that arise in sufficient quantities. One speaks of stage I, the so-called "Full compensation“Kidney disease in which a special diet is not yet required.
As the disease progresses, the urea and creatinine levels in the serum are primarily used as indicators for the beginning of a protein-restricted diet. With moderate renal impairment (compensated retention), a serum creatinine of 3 - 6 mg / dl and a urea value below 150 mg / dl, a protein intake of 0.5 - 0.6 g per kg of body weight is recommended. We recommend a lacto-vegetarian diet consisting of plant-based foods, milk and milk products.
Read more on this topic at: urea
As soon as the serum creatinine exceeds 6 mg / dl, a strictly low-protein diet with 0.35 g to 0.45 g protein per kg body weight is necessary in order to limit symptoms such as nausea, vomiting or loss of appetite and to increase the patient's quality of life. At this stage, the kidney's reduced ability to excrete can be positively influenced by an appropriate diet adapted to the creatinine levels and a balanced water balance.
Using the creatine and urea levels in the blood, the doctor can determine the progression of the disease and prescribe the necessary diet. This primarily results in a restriction of the protein intake with food. Essential amino acids are given in tablet form if required. The water and salt intake must be individually adapted to the loss of function of the kidney. There are several of these low-protein diets, all of which include a high-energy basic diet combined with a diet rich in essential amino acids. The best known forms of diet are the “potato and egg diet” according to Kluthe and Quirin and the “Sweden diet” according to Bergström.
Both types of diet are described in detail in the chapter “Practical nutritional therapy for chronic kidney failure”. End-stage chronic renal insufficiency (terminal renal insufficiency with a creatinine level of over 10 mg / dl in the serum) can only be controlled with the help of dialysis (blood washing) or transplantation. Separate diet forms are indicated for hemo- or peritoneal dialysis.
You can find more information about these diet forms under our topics:
- Potato and Egg Diet
- Sweden diet
Nutritional therapy for chronic renal failure / Theoretical principles
protein
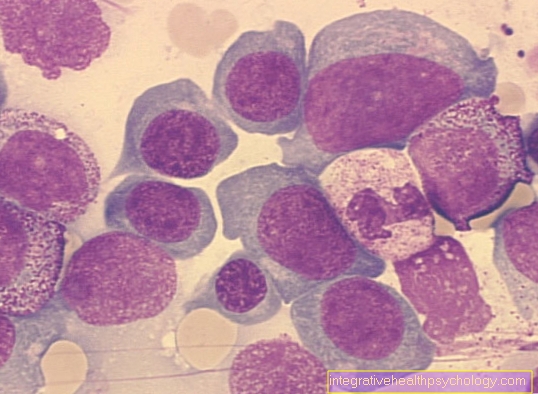
Protein is an important building material in our body and vital. We take protein from foods that contain protein like Meat, eggs, dairy and Dairy products and plant foods. The smallest building blocks of protein are the amino acids. There are some of these amino acids that the body cannot produce on its own and that we need to take in with our food to stay healthy. Your intake is necessary for the build-up of endogenous protein such as Muscles, Skin, all internal organs, hormones and digestive enzymes are absolutely necessary. The dietary protein, which we take in on average 70 to 100 g daily, is broken down into amino acids in the intestine and released into the blood. The amino acids are transported to wherever they are needed. Amino acids are also broken down in the body, on the one hand from excess food protein and on the other hand from body protein which is constantly being renewed. The end product of the metabolism is urea. This is excreted through the kidneys. If the organ is damaged to a certain degree, urea can no longer be excreted sufficiently and its concentration in the blood serum increases. This leads to further disturbances in the protein metabolism and patients complain of tiredness, nausea, vomiting and loss of appetite. At the same time, the concentration of other toxic substances also increases (for example creatinine) in the blood serum, which also come from protein metabolism. Keeping the blood urea level as low as possible is an important goal in the dietary treatment of chronic kidney failure. This is achieved by restricting the protein intake. However, there is always the risk that there will be an insufficient supply of essential amino acids. So you are faced with the problem of taking in just enough protein so as not to let the blood urea rise and on the other hand still supplying sufficient amino acids. This problem can only be solved if only foods with very high quality protein are used as protein suppliers. So only foods are allowed whose protein in the content of essential amino acids is sufficient (wholesome).
There is also the possibility of combining certain foods, as is the case, for example, with the potato and egg diet. With this type of diet there is the difficulty of the very limited choice of food. Other protein-rich foods like Meat fish and poultry practically have to be banned completely and so this form of nutrition can become too monotonous and stressful for the patient in the long run. Following this problem, Bergström developed the so-called "Swedish diet". At this "Protein balanced diet“The protein intake is of course also to be limited according to the severity of the kidney failure. However, all foods may be eaten within the permitted amount of protein, without having to pay attention to their value (content of essential amino acids).
The essential amino acids are supplied here in the form of medication, for example EAS oral tablets that are to be taken with meals. However, the high number of tablets sometimes causes problems. The granules with the same ingredients often cause an unpleasant aftertaste. The supply of amino acids can also take place with the help of their precursors, the so-called keto acids, which are available in the form of tablets, pearls or granules. These are mainly used in advanced renal insufficiency because they put less strain on the kidneys and produce less urea.
Carbohydrates and fats
In addition to the controlled protein intake, sufficient energy intake is of particular importance for successful diet therapy for kidney failure. If the calorie intake is insufficient, the body's own protein and the little dietary protein consumed are used for energy supply. There is an undesirable increase in urea. To ensure adequate energy supply, at least 35 kilocalories per kg of body weight should be consumed per day. Carbohydrates and fat serve as energy sources. When choosing fat, preference should be given to vegetable fats. For example, rapeseed oil, sunflower oil, corn oil and olive oil are recommended. Body weight loss must be prevented and regular weight control is advisable.
sodium
A limitation of sodium (Table salt) is generally not required for chronic kidney diseases. In kidney patients, however, there is often a retention of water and sodium in the body. As a result arise Edema (Water retention) under the skin and (or) in the vessels and a high blood pressure. In this case, a sodium restriction is necessary. The salt intake should not be more than 3 - 5 g per day. This can be achieved by using table salt very sparingly when preparing meals, and under no circumstances "add salt" to the recommendation at the table. Highly salty foods must be removed from the menu.
Sodium is rarely depleted due to salt loss through the kidneys or diarrhea and vomiting. In this case, more salt and liquids have to be taken in with the food. In the case of higher salt losses, sodium can also be given with the help of an infusion. The salt intake in chronic kidney failure can vary greatly from person to person.
potassium
With minerals potassium the permitted intake also varies from case to case. With advanced renal insufficiency, life-threatening hyperkalemia (potassium levels in the blood serum above 6 mmol / l) can develop. To avoid this, foods rich in potassium must be removed from the menu.
Foods very high in potassium and not suitable:
- Bouillon cubes, meat extract, low-salt sausage, meat and fish preserves, stockfish.
- Broccoli, spinach, fennel, mushrooms, kale, peas, corn, chard, tomatoes, legumes, sprouts and sprouts, tomato ketchup, tomato paste and vegetable juices.
- All kinds of potato products.
- Apricots, banana, kiwi, avocado, honeydew melon, fruit juices, dried fruits of all kinds, nuts and seeds.
- Whole grain products (crispbread, whole grain bread in large quantities, pumpernickel, bran, grains, cereal flakes, muesli, muesli mixes), whole grain rice, whole grain pasta.
- Chocolate and all sweets made with chocolate.
- Cocoa and beverages containing cocoa
- Potassium-based table salt substitute.
Suitable foods
- Fresh meat, fresh fish and fish products of all kinds up to 120 g per day
- Sausage products of all kinds, preferably liver sausage, mortadella, sausage
- All sorts of milk and milk products
- Fats preferred vegetable oils for cooking and for salads, butter
- 1-2 eggs a week
- 1 no portion of lettuce daily (30g) and up to 200 g vegetables (not high in potassium!), 150 g potatoes
- 150 g cooked fruit (not high in potassium!) Without liquid.
- 100 g fresh apple, pear, watermelon or 200 g fresh blueberries or cranberries.
- White bread, brown bread, toast bread, rusks, wholemeal bread in small quantities
- (30 g daily), rice, pasta, semolina, corn flakes.
- Any amount of sugar and candy without chocolate.
- Malt coffee, tea, lemonade. Coffee, wine and beer in small quantities.
- Water, mineral water (with sodium restriction, sodium content below 20 mg per liter)
All spices (pay attention to the salt intake if sodium is restricted and never use salt substitutes with a high potassium content!), Fresh herbs only in very small quantities.
For potatoes, vegetables and frozen vegetables that are permitted and suitable within the framework of the diet plan, the potassium content can be reduced by 2/3 by chopping them up, then soaking them in water (24 hours) and pouring off the cooking water several times. The vitamin losses with this type of preparation are due to the ingestion of water-soluble Vitamins (vitamin C and B vitamins) in tablet form
A Hypokalemia (Potassium levels in the blood serum too low) occurs in cases of chronic kidney failure (chronic kidney failure) only in exceptional cases. It often manifests itself in muscle cramps and can be positively influenced by a diet rich in potassium. Effervescent tablets can also be used.
Phosphate and calcium
In the chronic kidney failure changes occur in the Mineral balance from Calcium and phosphorus on. The Creatinine level 3 - 5 mg / dl in the serum above an, phosphorus is excreted less via the kidneys and the blood level rises. As a result, the calcium level in the serum can drop (hypocalcaemia). Bone metabolism disorders and long-term bone diseases occur.
Therefore should the daily phosphate intake with food on 1g limited become. All phosphate-rich foods must be removed from the menu. In the case of moderate renal insufficiency, this measure is sufficient to keep the phosphate level at normal.
Unsuitable phosphate-rich foods
- Processed cheese, Camembert, Emmentaler, Edam, Chester, milk powder.
- Oil sardines, smoked halibut
- Wheat bran, wheat germ, oat flakes, wheat germ, brown rice, crispbread, whole wheat bread
- Porcini mushrooms (dried), legumes.
- Peanuts, Brazil nuts, walnuts, almonds
- Cola drinks
- Food with added phosphate such as sausage products.
In addition to these dietary recommendations, it may be necessary to lower the phosphate level with medication.
With minerals Calcium Inadequate absorption can occur in the early stages of kidney failure. The protein-reduced form of nutrition that Renal failure is necessary excludes an increased intake of calcium. The most important calcium-rich foods are milk and milk products, which have to be restricted due to their high protein content. Calcium must therefore be supplied in the form of medication.
Vitamins
In the context of a protein-reduced diet, the supply of vitamins is often insufficient B vitamins and Vitamin D is often insufficient. The B vitamins are primarily missing that Vitamin B6 and the Folic acid. The administration of all water-soluble vitamins in tablet form has proven itself here. The administration of vitamin D is necessary if the renal osteopathy (increased bone loss) continues despite a low-phosphate diet and the administration of calcium-containing phosphate binders in tablet form. In a diet low in potassium, which requires certain foods to be soaked, the water-soluble vitamins C and B are always missing. In contrast, the vitamin A level is often increased in the case of chronic kidney failure and intake is not appropriate.
Trace elements
An intake of iron can also be necessary if the diet is low in protein. In the case of existing complaints (for example impotence) the trace element zinc must also be given in tablet form.
Amount of liquid
While with moderate impairment of the kidney function 2 - 3 liters per day should be drunk in order to remove the urinary substances, the ability of the organ to excrete sufficient fluid decreases as the disease progresses.
This course is very different from patient to patient. The goal is to avoid overhydration at this stage because it can be life threatening Pulmonary edema could lead. The permissible amount of liquid depends on the medical prescription. The basic rule for the permitted amount of liquid is: Amount of urine excreted the day before plus 500 ml.