Local anesthesia
introduction
Local anesthesia is local anesthesia by switching off pain in nerves and conduction pathways without impairing consciousness.
The local anesthetic is always reversible and can be used for surgical interventions and painful examinations as well as for pain therapy.
Duration of anesthesia
The duration of a local anesthetic can vary widely. The decisive factor here is the amount, substance and concentration of the drug that is used for anesthesia.
For fingers and toes, the amount of anesthetic is limited to 4 ml, as otherwise the blood circulation in the fingers could be disturbed. The effect ends on average between 2 and 16 hours through the breakdown and removal of the anesthetic in the blood and through distribution into the surrounding tissue.
The effect slowly wears off and the sensations such as pain and temperature gradually come back.
With such procedures under local anesthesia, it is important to be prepared for the return of pain after the procedure, despite the initial freedom from pain, and to have sufficient pain medication on hand or, if necessary, to have them prescribed by the doctor.
How long a local anesthetic works depends on which drug is used. The substances also differ in their onset of action. For example, with lidocaine, a very common local anesthetic, there is no pain in the area of application within a few minutes. Afterwards it works for about one to two hours.
Bupivacaine, another local anesthetic, works for two to five hours, but takes a little longer before the effect occurs after the injection.
Side effects of local anesthesia
Important side effects of local anesthetics are allergic reactions and disorders of the central nervous system and the cardiovascular system.
In the context of allergic reactions, symptoms can appear on the skin (e.g. urticaria, so-called hives) or on the whole body, in the sense of asthma attacks, bronchospasm and a drop in blood pressure. In the worst case, anaphylactic shock with cardiac arrest can occur.
These side effects occur mainly with local anesthetics of the ester type, which are rarely used today.
Influencing nerve cells can lead to a typical metallic taste, and sensory disturbances in the area of the mouth and tongue are also possible.
Other side effects include restlessness and muscle twitching, up to seizures, as well as changes in speech, sight and hearing.
Higher doses can lead to respiratory paralysis and cardiac arrest. With regard to the cardiovascular system, a slowed heart rhythm and disturbances in the conduction of excitation in the heart can occur. These can be reasons for a drop in blood pressure and cardiac arrest.
Read more on the subject at: Side effects in local anesthesia
Regional anesthesia procedure
There are different ways to perform local anesthesia:
- Surface anesthesia:
In this method of local anesthesia, the superficial nerves are numbed by applying a local anesthetic to the skin or mucous membrane. The drug can be applied to the affected area in the form of sprays, powders, solutions or ointments.
- Infiltration anesthesia:
In the course of infiltration anesthesia, the anesthetic drug (local anesthetic) is injected into the region to be anesthetized with the help of a needle. After a short waiting period, the anesthetic will work and the treatment can be carried out.
Depending on the puncture site and pain sensation, injecting the drug can be uncomfortable or painful.
This form of local anesthesia is a very frequently used and uncomplicated type of anesthetic.
- Anesthesia near the spinal cord:
These include the so-called spinal anesthesia and epidural anesthesia (also called epidural anesthesia / PDA). In both procedures, the nerve fibers are blocked directly at their exit point from the vertebral bodies. That is why one speaks of a central nerve block.
The main areas of application for these procedures are operations on the legs up to the groin, as well as obstetric or urological interventions.
The complications of anesthesia close to the spinal cord are minor. However, an incorrect injection of the drug can cause problems.
Depending on the injection site, paralysis of the respiratory muscles and, as a result, a subjective feeling of shortness of breath can occur.
In addition, particularly with strong anesthesia, pronounced vasodilation can occur, as a result of which cardiac output and blood pressure decrease sharply. This can be prevented or treated by adding volume and plenty of fluids prior to anesthesia.
Headache may occur after treatment. The exact cause of this is unclear; experts are discussing headaches as a result of a loss of liquor or as a result of inflammatory cranial nerve irritation. On the other hand, lasting neurological damage is very rare.
Since the patients are awake and fully conscious during regional anesthesia, it is important to explain the exact processes beforehand.
Read more on the subject at: Regional anesthesia
Spinal anesthesia
In spinal anesthesia or local anesthesia, the anesthetic is injected into the liquor space near the spinal cord. To avoid injuries to the spinal cord, the anesthetic is injected below the 3rd lumbar vertebra.
Since the human spinal cord grows more slowly than the vertebral bodies, in the area below the 1st lumbar vertebral body there are usually only the nerve roots in the liquor.
In order not to injure the spinal cord under any circumstances, the anesthetic should be injected into the L3 / 4 intervertebral area.
The puncture of this local anesthetic can be performed with the patient sitting or lying on their side.
There are then two options for anesthesia:
- Single injection:
A dose of anesthetic is injected directly and the needle is then removed again.
- Indwelling catheter:
After the anesthetic is injected, the needle is not removed. Instead, a thin plastic catheter is inserted over the needle into the liquor space. The catheter remains in the cerebrospinal fluid space so that you have the option of administering a new dose of local anesthetic at any time.
The advantage of a lying catheter is the possibility of re-injection during operations and postoperative analgesia.
The drugs are usually heavier than the CSF and therefore spread depending on the position.The anesthetic can be controlled via the patient position, but also via the height of the injection site and the amount and density of the anesthetic.
Read more on the subject at: Spinal anesthesia
epidural
Epidural anesthesia is also one of the spinal cord-related anesthesia of local anesthesia. In contrast to spinal anesthesia, the anesthetic is not injected directly into the liquor space, but into the dura space.
Since the anesthetic has to diffuse through the hard meninges before it takes effect, it takes 20-30 minutes before anesthesia occurs.
In addition, more anesthetic has to be injected. As with spinal anesthesia, the anesthetic is injected into the L3 / 4 intervertebral space.
However, it can also be carried out in the other areas of the vertebrae, as the CSF space is not pierced directly and there is therefore no danger to the spinal cord.
Nevertheless, the correct position of the catheter / needle should be checked after the puncture in order to rule out a spinal position. The dose of anesthetic that is given during epidural anesthesia can be up to 5 times as high and, if incorrectly positioned, would lead to spinal anesthesia that is much too strong.
Indications for epidural anesthesia are long-term interventions, longer postoperative pain therapy and obstetrics.
Peripheral nerve block
In addition to anesthesia close to the spinal cord, there is also the option of peripheral nerve blocks. The anesthetic is injected in the immediate vicinity of the nerve plexus or individual nerves, thus enabling anesthesia that is limited to the surgical area.
The advantage of such local anesthesia is a low rate of complications compared to general anesthesia.
Read more on the topic: Anesthesia complications
Nevertheless, side effects can certainly occur because relatively large amounts of local anesthetic have to be injected. This can lead to side effects in the brain or on the blood vessels and heart. It is therefore important to inject the anesthetic slowly in small doses in order to identify possible side effects of this local anesthetic at an early stage.
Read more on the subject at: Local anesthesia side effects
The risk of nerve damage is low, as special atraumatic needles are used and the position of the nerves can be precisely determined with the help of an ultrasound device or a nerve stimulator. It is also possible to use an indwelling catheter with peripheral anesthesia.
This enables postoperative pain management and longer surgery.
The tumescent local anesthesia
Tumescent local anesthesia, which was developed in plastic and reconstructive surgery, is used to numb large areas of the body without general anesthesia. Tumescent local anesthesia (TLA) is a regional anesthesia in which large amounts of a previously diluted local anesthetic are infiltrated into the skin and subcutaneous fatty tissue. In addition to anesthesia over a large area, this also leads to severe swelling of the tissue, hence the name tumescent anesthesia ( tumescere = to swell).
The main area of application for tumescent local anesthesia is liposuction. The specialty of this form of anesthesia is used to remove large amounts of fat without the need for general anesthesia. The local anesthetic solution used is usually a mixture Sodium chloride water and the local anesthetic Lidocaine. In order to keep blood loss as low as possible, even during major operations, adrenaline is usually added. adrenaline causes a narrowing of the blood vessels, which leads to less blood flow and thus less blood loss in the surgical area.
Further information on the subject can be found here: The tumescent technique
Local anesthetic poisoning
Intoxication (poisoning) with local anesthetics can occur, for example, if the drug gets directly into the bloodstream instead of into the tissue. The central nervous system can react with restless states, muscle tremors and cramps, but also dizziness, nausea and vomiting.
A metallic taste may appear in the area of the tongue and sensory disturbances may occur. With more severe intoxication, the heart is weakened and the blood pressure drops. The heart rhythm can also be slowed down, which can lead to cardiac arrest.
There are seldom allergic reactions, especially due to the now rarely used local anesthetics of the ester type.
These can manifest themselves in the form of skin symptoms such as itching and hives, asthma attacks and anaphylactic shock with circulatory failure.
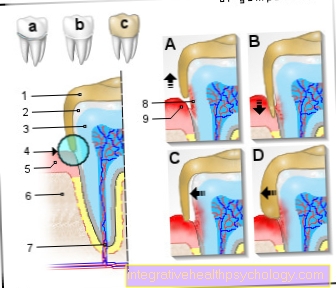
Local anesthesia at the dentist
At the dentist, most procedures are only performed under local anesthesia. Common means such as lidocaine, to which adrenaline is added, are used for this.
Adrenaline prolongs the effect of the local anesthetic and reduces bleeding. Local anesthesia is recommended in the oral cavity, as a numbness in the treatment area can be achieved with the help of less targeted injections. Depending on the treatment, a syringe with the local anesthetic is inserted into the gums or to the bone in order to inject the drug there.
The anesthetized nerves and their branches then no longer transmit pain impulses to the brain. The duration of action and therefore freedom from pain is between one and five hours, depending on the type of anesthetic. Apart from a possible brief pain when giving the syringe, patients do not feel any pain during dental interventions.
The local anesthetic procaine is also often used in dentistry. Please also read our article on this: Procaine syringe
Read more on the subject at: Line anesthesia at the dentist, Local anesthesia at the dentist,
Local anesthesia for arm and shoulder injuries
For anesthesia of the shoulder and the arms, different options of local anesthesia are possible:
- Brachial plexus anesthesia:
The axillary access in brachial plexus anesthesia (Local anesthesia) is the simplest form of anesthesia in the shoulder area.
The anesthetic is injected near the artery in the armpit area.
Since the artery can be felt very well, no ultrasound control or nerve stimulation is required.
However, the nerves do not all converge in this area, which is why a single puncture site is not definitely sufficient to numb the entire arm.
This procedure enables operations in the area of the lower arm and hand.
Contraindications for such a blockage are previous damage to the Brachial plexus, an inflammation of the lymphatic system in this area, as well as a previous breast removal with removal of the lymph nodes.
- Vertical Infraclavicular Block:
Another possibility of local anesthesia in this area is the so-called vertical infraclavicular blockade, which also allows interventions on the upper arm.
It is pierced below the collarbone.
To avoid the risk of lung injury, the puncture is performed under ultrasound control or with the help of a nerve stimulator.
Due to the localization, there is also a risk of the axillary artery.
Since hemostasis is difficult in this case, the patient's coagulation must not be impaired.
Other contraindications are pulmonary dysfunction and paralysis of the N. phrenicus the other side. This innervates the diaphragm and would lead to respiratory insufficiency in the case of bilateral paralysis, as the diaphragm is the main breathing muscle.
- interscalene blockade:
The third possibility of anesthesia in this area is the interscalene block. The puncture site is above the collarbone and therefore allows shoulder surgery.
Due to the large number of important arteries and nerves running close by, precise control of the puncture by ultrasound or nerve stimulation is a prerequisite for performing such anesthesia.
These location conditions therefore also require the function of the corresponding nerves on the other side. Because here, too, the diaphragmatic nerve can be paralyzed and thus make breathing impossible.
Also the so-called Recurrent nerve runs in this area. It is responsible for opening the glottis and leads to hoarseness in unilateral paralysis.
However, if the nerve is paralyzed on both sides, the glottis is closed and thus hinders breathing.
Pulmonary dysfunction is also a contraindication for such anesthesia. Furthermore, with this local anesthesia there is a risk of injection into the A. vertebraliswhich supplies the brain with blood and can therefore lead to extremely toxic reactions and seizures when anesthetics are administered. An injection into the epidural or spinal space would be similarly dangerous.
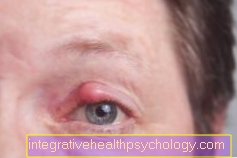
Local anesthesia on the eye
In contrast to other parts of the body, the eye is very easy to numb locally, which is necessary for almost every operation on the eye and is also carried out by default.
For children and in other special cases, however, general anesthesia is recommended for this type of procedure.
For simple interventions, there is an anesthetic in the form of a gel or eye drop, which is applied to the eye and makes the operation possible. This type of anesthesia is perceived by the patient as very pleasant and uncomplicated and carries hardly any risks for the patient.
If deeper interventions are necessary on the eye, an anesthetic of the eyeball may be necessary after the local anesthesia described above. Here, the eyeball is anesthetized with a syringe in two places on the side of the eyeball.
This type of anesthesia with the syringe is performed either under short or local anesthesia and in some cases can be uncomfortable for the patient.
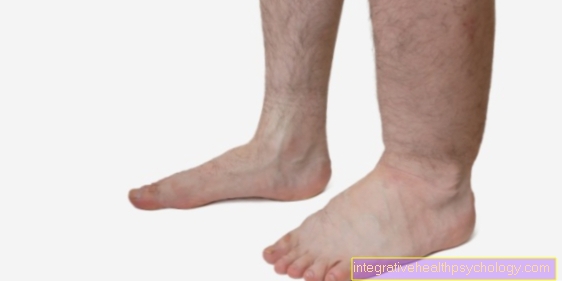
Local anesthesia on the finger
Fingers are very well suited to be anesthetized individually. The standard procedure is the so-called Colonel conduction anesthesia.
Four nerves run in the fingers that report sensations such as pain and temperature from the finger to the brain. They are located in pairs on the top and bottom of the fingers, on the right and left of the finger bone.
By injecting anesthetic around the bones, these nerves are numbed and can no longer transmit the pain to the brain and the patient can no longer feel it and interventions on the finger are painless.
Toes can also be anesthetized very well with this procedure, since the nerves run around the bones here just like on the fingers. After the injection, it only takes a few minutes and the finger begins to go numb until it is finally completely numb.
Before the doctor's intervention begins, there is always another check to see whether every feeling has actually disappeared.
Mobility is not impaired by the anesthetic and is still possible, as many of the muscles that move the fingers are located in the forearm and are only connected to the fingers by long tendons.
Local anesthesia on the ear
Local anesthesia is also often used for operations on the ear. In addition to injuries, the focus here is also on the use of cosmetic surgery to put on the ears in classic "sail ears". The anesthetic is done by injecting the anesthetic behind the ears.
Typical patients who decide to have their ears big are mostly school-age children, but also adults. In children, local anesthesia should be viewed critically, as children could be traumatized by an operation so close to the face and they cannot lie without movement for so long.
An operation under local anesthesia would be extremely stressful for children. For this reason, a stress-free general anesthetic is used here.
For adults, local anesthesia is the first choice if the patient is confident enough to perform the procedure while they are conscious.
If you decide not to experience the procedure so close to the face with full consciousness, a slight immobilization or a twilight state can be achieved through medication and the additional local anesthesia will not immediately require general anesthesia with ventilation.
The advantage is that after a pure local anesthetic, you can be released home after a short break. Here, too, you should definitely remember to have enough painkillers on hand for the onset of pain after the local anesthetic.
Since the ear is a very sensitive organ, operations on areas inside the ear or middle ear can often only be performed under general anesthesia.
Local anesthesia during pregnancy
Even if anesthesia should always be carefully considered during pregnancy, there are situations in which local anesthesia is absolutely necessary. These include injuries that have to be stitched up or urgent dental operations that cannot be postponed until after delivery. (please refer: Local anesthesia in dentistry)
Even if local anesthesia is considered to be very safe and low-risk for the unborn child, there are some special features that should be observed in order to minimize the risk to the child.
In any case, it is important to inform the attending physician about the pregnancy so that he can observe these particularities.
Surgery under local anesthesia can be performed at any time during pregnancy. In contrast, general anesthesia should not be used in the first few months of pregnancy.
When it comes to the choice of anesthetic drug, however, there are differences to non-pregnant women. The usual drugs (= Anesthetics) are very fat-soluble and can easily pass through the umbilical cord into the child's circulation, but larger amounts should get into the bloodstream under local anesthesia, which is actually not intended. Here anesthetics should be chosen that are not so easily soluble in fat and, in the worst case, do not get into the child's circulation, since anesthetics should get into the bloodstream.
Medicines are usually mixed in with the remedies, which constrict the blood vessels. This is to prevent the drug from spreading excessively and causing major bleeding.
This should be on in pregnancy Adrenaline descendants be resorted to, as some other substances can cause labor.
However, if you take all these peculiarities into account, there is usually nothing in the way of interventions under local anesthesia. If a great fear of such interventions still plays a role, tranquilizers can also be used here.
The Benzodiazepines As the diazepam has been proven and can also be used briefly during pregnancy with a clear conscience to dampen the stress reactions of the expectant mother, which are also noticeable for the child.
Is local anesthesia possible during breastfeeding?
Local anesthesia or local anesthesia is generally possible during breastfeeding. However, breastfeeding should be discussed with the attending physician in advance in order to choose the right local anesthetic. The greatest experience with local anesthetics during breastfeeding is with Articain, Bupivacaine and Lidocaine. These substances can be applied locally in small concentrations without hesitation, without them being excreted in breast milk and harming the baby.
Effect of local anesthesia
Local anesthesia is a method of local anesthesia and has no addictive or euphoric effect.
All local anesthetics work in the cells and block sodium channels there. When the cell is excited, sodium flows through these channels out of the cell and depolarizes the cell. This depolarization then excites the next cell and the signal is transmitted via the nerves to the brain.
If these channels are blocked, there can be no transmission of the stimulus. This blocks the sensation of pain in the numbed area.
Depending on the dosage of the anesthetic, the potassium channels in the cells can also be blocked. This also leads to the elimination of pressure and temperature sensations.
In addition to switching off sensitive sensations such as pain and temperature, the motor skills can also be anesthetized, so that mobility in certain muscle groups becomes impossible for some time.
Local anesthesia in a cream
There are a number of creams that additionally contain a local anesthetic such as Lidocaine or Xylocaine are offset to one short-term local anesthesia of the skin to reach. The use of anesthetic creams is varied and ranges from prophylaxis to painless blood sampling in children, to relieve pain and discomfort in skin infections. Anesthetic creams are also very popular in the private sector, for example for numbing the skin before hair removal or local anesthesia before a piercing or tattoo is done.
Dentinox® teething gel
Dentinox® is a gel that is used to aid teething in babies. Most children have milk teeth when they are around half a year old. This is a painful process for some children and a correspondingly exhausting time for parents. To make the teething process easier for children, Dentinox® gel contains a mixture of anti-inflammatory chamomile tincture and a local anesthetic that relieves pain Lidocaine. Regular application of Dentinox® gel should facilitate the teething process by reducing pain.
You might also be interested in: My baby is sleeping poorly - what can I do?
Summary
Local anesthesia has many advantages and is now widely used due to its low complications.
The patient is awake and responsive and the stress on the entire circulatory system is significantly lower than with general anesthesia.
However, it is important to be careful with these substances, as they can lead to severe and life-threatening complications if the wrong injection or dosage is used.
For this reason, it is important to check the exact location of the nerves and nearby structures with the help of imaging.
The main areas of application for local anesthesia are operations in certain areas, obstetrics and long-term pain therapy. In the course of time, various methods of anesthesia have been developed that make a very precisely localized anesthesia possible.