Nerve inflammation
introduction
A nerve inflammation (Latin: neuritis) describes the inflammation of peripheral nerves or cranial nerves. If only a single nerve is affected it is called mononeuritis, if several nerves are inflamed it is a polyneuritis or polyneuropathy. The symptoms of nerve inflammation depend entirely on which nerve is affected and how badly it is.

Overview of the causes of nerve inflammation
There are different causes of nerve inflammation. These include:
- viral or bacterial infections
- traumatic injuries from accidents
- Toxins (poisonous substances) such as alcohol or drugs
- Harmful metabolic products
- Autoimmune disease such as Guillan-Barré syndrome
- Pressure on nerves such as a herniated disc
Multiple sclerosis (MS) is a chronic form of nerve inflammation. Here, too, the myelin sheaths of the nerves are attacked, but in the central nervous system, i.e. in the brain and spinal cord tissue.
In principle, any nerve can be affected by an inflammation of the nerves, which is why the symptoms vary depending on which function the respective nerve can no longer fulfill.
therapy
Nerve inflammation is treated differently depending on its type and cause. If there is an underlying infection, antibiotics or antivirals can help.
Is there a compression syndrome such as In the case of a herniated disc or carpal tunnel syndrome, surgical therapy may be necessary. In general, nerve inflammation can also be treated with pain relievers. Physical applications such as physiotherapy, warmth or cold and massages can also help relieve symptoms. Acupuncture is also used as an alternative treatment method.
When do you need cortisone?
Cortisone develops its effect, among other things, by inhibiting certain mechanisms of the immune system. That is why almost all autoimmune diseases are cortisone applications.
In the area of nerve inflammation, this applies above all to multiple sclerosis (MS) and CIDP, a chronic form of Guillain-Barré syndrome. In MS, cortisone is the first choice for treating acute relapses. For almost all other nerve inflammations, other therapeutic approaches should first be selected and cortisone should only be used if these have not achieved a satisfactory effect. This is due to the fact that long-term use of cortisone can cause a variety of side effects, such as Osteoporosis or an increase in blood sugar and fat levels.
Home remedies for treating nerve inflammation
First of all, it should be emphasized that home remedies for diseases such as multiple sclerosis or Guillain-Barré syndrome can of course only be a supplement to the established, scientifically founded therapies.
The best home remedies for a nerve inflammation include warmth on the affected body regions, for example in the form of hot water bottles or cherry stone pillows. In addition, physiotherapy and massages can also be helpful, especially with inflammation of the nerves in the back and neck area.
Some people also report that putting on cabbage wraps (either with cabbage or savoy cabbage) gives them relief. Others report improvements from taking ginkgo biloba or drinking St. John's wort tea.
In addition, those affected should eat a balanced diet that is particularly rich in B vitamins: Whole grain products, lentils and dairy products, for example, are good sources of vitamin B6. The latter also contain plenty of vitamin B12, as do fish and meat.
homeopathy
In addition to the conventional medical treatment approaches described above, homeopathy also promises help for those affected by nerve inflammation. The most common are Hypericum perforatum (St. John's Wort), Aranea diadema (extract of the garden spider), Gnaphalium (Ruhr herbs) and Kalium phosphoricum (Schüssler Salt No. 5) are recommended.
In this context, however, it should be noted that there is no scientific proof of the effectiveness of homeopathic remedies and that an effect beyond the placebo effect is considered to be virtually excluded from a logical point of view. It should therefore be emphasized that for people who believe in homeopathy, although it is a worthwhile addition to the established medical treatment strategies, it must by no means be regarded as a substitute for them!
Duration of an inflammation of the nerves
Since the spectrum of diseases that can be associated with nerve inflammation is very broad, no general statement can be made about the duration of nerve inflammation. While the duration of the Guillain-Barré syndrome as an example of acute nerve inflammation can be estimated at a few weeks to a few months, for example, multiple sclerosis is an incurable disease and accompanies those affected for a lifetime.
In the case of vestibular neuritis, most patients are symptom-free after about 6 to 12 weeks, even if the function of the organ of equilibrium can still be determined over a longer period of time with the aid of technical examinations.
Regardless of its cause, however, the following generally applies: An early start of treatment and consistent compliance with the therapy guidelines can in most cases have a significantly positive effect on the duration of the nerve inflammation. So do not hesitate too long to go to the doctor if you experience symptoms and make sure that you take the prescribed medication regularly or attend physiotherapy appointments.
Read more on the topic: Duration of an inflammation of the nerves - what you should be aware of!
Nerve inflammation on the head
There are many nerves in the head area that can be affected by neuritis.
The cranial nerves that can become inflamed include, for example, the optic nerve (lat: Optic nerve). One then speaks of optic neuritis.
The main symptoms of this nerve inflammation are visual disturbances (deterioration in visual acuity, in the worst case blindness) and pain, especially when moving the eyes. Depending on the cause of the inflammation, the symptoms appear on one or both sides. If it is one-sided, it is usually an extension of a local inflammation (e.g. inflammation of the paranasal sinuses or the retina of the eye) to the optic nerve. If the symptoms appear in both eyes, the causes are more complex. Optic neuritis can be autoimmune and occur in the context of other diseases such as multiple sclerosis (MS), vasculitis (inflammation of the blood vessels) or systemic lupus erythematosus (SLE). Bacterial or viral systemic diseases (syphilis, Lyme borreliosis), the infectious disease toxoplasmosis in the case of immunocompromised, poisoning with alcohol, nicotine, lead or thallium or certain drugs can manifest themselves in optic neuritis. The prognosis for optic neuritis is usually good and it is treated with glucocorticoid therapy.
Read more on the topic: Optic nerve inflammation
The nerves that are responsible for eye movement can also become inflamed as part of an autoimmune process (for example in Guillain-Barré syndrome). This can result in oculomotor paresis, i.e. paralysis of the eye muscles in which the mobility of the eyeball is reduced. Other possible symptoms are a drooping upper lid, a rigid, wide pupil and accommodation disorders (“focusing” is disturbed).
If the part of the auditory and equilibrium nerves that is responsible for balance is inflamed, it is called vestibular neuritis. This can be caused by a virus infection or reactivation (e.g. with herpes viruses). Another cause is a circulatory disorder of the balance organ. Typical symptoms are vertigo and vomiting.
The part of the auditory and equilibrium nerves that is responsible for hearing can be affected by toxins produced by bacteria - e.g. syphilis, scarlet fever, typhus, diphtheria, measles - or other substances (tobacco, alcohol, heavy metals).
Nerve inflammation in the neck
In the case of nerve inflammation in the neck, the symptoms are usually based on tension in the neck muscles. The tense muscles force an unnatural and unhealthy neck posture, which irritates the nerve tracts in the neck and can lead to pain in the neck and also to headaches.
The cause of the tension in the neck muscles is in most cases too long sitting on unsuitable seating surfaces, for example in the office. For most of those affected, improving the sitting conditions and taking regular breaks from sitting with physical exercises are very effective measures to alleviate symptoms.
As long as it does not become the norm, it can occasionally be useful to take a painkiller to relieve the pain, thereby loosening the tension and thus breaking the cycle of pain and tension.
Nerve inflammation of the cervical spine
Inflammation of the nerve roots can occur in the entire spine. A nerve root is the union of sensory and motor nerve fibers on the side of the spine. It can be irritated by infections or pressure. Nerve root inflammation is also called radiculopathy.
Pressure damage can be caused by arthritis (ossification of the intervertebral hole, exit point of the spinal cord nerve from the spinal cord) or due to a displacement of the intervertebral discs. In the case of a herniated disc in the cervical spine (Cervical spine), parts of a disc enter the spinal canal and press on the nerve roots. The nerves that lead to the arm are compressed.
This can lead to pain that radiates from the cervical spine into the arm. In addition, numbness (especially in the fingers) and symptoms of paralysis can occur. In rare cases, a tumor can also be responsible for the compression of the nerve root.
Nerve inflammation on the face
The facial nerve (nervus facialis), which innervates the facial muscles, can be damaged by infectious diseases, mechanical trauma (e.g. petrous bone fracture), but also by cerebral haemorrhages or tumors.
In the case of infections, this leads to inflammation of the facial nerve. Then it comes to failure symptoms. These are mostly paralysis of the facial muscles on the affected side and disorders of taste perception.
Another form of nerve damage on the face is trigeminal neuralgia. It can occur as part of multiple sclerosis, but the cause is often unclear. In trigeminal neuralgia, the fifth cranial nerve is in a state of irritation that is very painful for patients. You suffer from sudden unilateral severe pain in the face that lasts for a few seconds. The pain usually occurs along the upper or lower jaw, as two of the three large branches of the trigeminal nerve run along there.
Read more about the topic here: Nerve inflammation on the face.
Nerve inflammation in the tooth
A tooth nerve can become inflamed when bacteria get to the nerve through deep caries. External stimuli such as pressure (due to fillings that are too high) or heat (e.g. when drilling) can damage the sensitive tooth nerves.
The painful inflammation of the dental nerve can be stopped with early treatment, otherwise the nerve can also die.
Nerve inflammation in the hand
If symptoms of nerve inflammation occur in the hand area, for example sensory disturbances (tingling), muscle weakness or pain, then one should think about the possibility of carpal tunnel syndrome. The median nerve is pinched, the nerve that is responsible for the feeling of the palm of the hand from the thumb to the inside of the ring finger and which, among other things, innervates the muscles of the ball of the thumb. In the case of a carpal tunnel syndrome, this can be reduced by the impaired function of the nerves. In the early stages of therapy, splints and pain relievers and anti-inflammatory drugs are used. If conservative therapy is unsuccessful, surgical decompression may be necessary.
Find out more about the topic here Nerve inflammation on the arm
Inflammation of the nerves in the elbow
A nerve pulls at the elbow (Ulnar nerve) on the inside of the arm between the tip of the elbow and the bone process of the humerus through the so-called cubital canal. This nerve innervates some muscles on the forearm (finger flexor muscles) and on the hand. It also sensitively innervates the skin on the side of the little finger on the hand.
If the nerve is compressed at the narrow point on the elbow, for example through long-term support of the elbow, bony changes or local growths of the nerve tissue, the picture of an "ulnar channel syndrome" / "cubital tunnel syndrome" can occur. Symptoms are numbness on the fourth and fifth fingers, the edge of the hand and the inside of the forearm. Later on, pain in the elbow that radiates into the forearm and hand can occur.
Finally, the muscles of the hand can be paralyzed, which manifests itself in difficulties with “pointed grip” (writing, opening a bottle). The cubital tunnel syndrome is comparable to the carpal tunnel syndrome on the wrist and is treated according to the same principle.
Nerve inflammation in the foot
The nerve damage that occurs on foot make noticeable belongs to the diabetic neuropathy. At Diabetics with badly adjusted Blood sugar toxic metabolic products are stored in the nervous tissue after a long period of time with increased blood sugar. This causes the nerves to lose their function. Often this nerve degeneration begins in the feet and rises symmetrically. It comes to Misalignments of the feet and thus to Incorrect loads and wounds. Since pain perception is also impaired, the wounds are often not noticed at first. These symptoms are referred to as "diabetic foot" summarized.
Another cause of a "diabetic foot" is through arteriosclerosis Reduced blood supply to the foot due to the leg vessels.
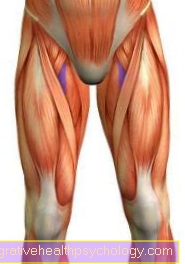
Inflammation of the nerves in the thigh
The skin of the thigh is supplied with sensitive nerves from the lumbar plexus. If one of these nerves is damaged, the typical symptoms of nerve inflammation in the thigh area and pain in the thigh can occur. Most of the time, there is also pain in other parts of the body. A lesion of the genitofemoral nerve hurts the upper inner thigh and leads to pain in the groin and in men the testicles, in women the labia majora.
Sciatic nerve pain occurs on the back of the thigh, lower leg and / or foot.
If the femoral nerve is damaged, there is a loss of sensitivity on the front of the thigh. In addition, motor failures can occur, whereby the hip can no longer be bent and the knee can no longer be straightened.
If only thigh pain is present without any other symptoms, a disorder of the obturator nerve can be considered. This leads to pain in the lower part of the inner thigh. Possible causes are compression or damage to the nerves in the context of a herniated disc, a pelvic fracture or other processes in the pelvis.
The sole pain or sensory disturbances on the outside of the thigh and on the anterior upper iliac spine can result from a lesion of the lateral femoral cutaneous nerve. This clinical picture is called meralgia paraesthetica, in which the nerve under the inguinal ligament is compressed.
More on this topic: Inflammation of the nerves in the thigh
Inflammation of the nerves on the ribs
Shingles is typical of an inflammation of the nerves that spreads along the ribs (Herpes zoster). This is based on an infection with the varicella-zoster virus, the primary disease of which is chickenpox (Varicella) triggers. After that, the virus remains inactive in the body in the nerve nodes for years.
If the immune system is weakened (which often applies with increasing age), the virus can multiply again. Then the viruses spread along the nerves again, which manifests itself in reddening of the skin with or without blistering and often severe pain in the affected area. In the area of the trunk there is a unilateral belt-shaped expansion.
Inflammation of the nerves on the back
If there is an inflammation of the nerves in the back, the complaints are usually expressed calmly. For example, getting up in the morning is felt to be particularly painful, and some people affected even wake up at night due to the pain. Physical activity, on the other hand, often alleviates the symptoms. If this is the case, nerve inflammation is much more likely than other causes, such as Arthrosis (wear and tear of the joints) or osteoporosis, in which the pain decreases when you are at rest and increases with physical activity.
In most cases of nerve inflammation in the back, the lower part of the back is affected, especially the sacrum joint. The expert then speaks of sacroiliitis. Such inflammations can occur individually or in combination with so-called rheumatic spondylarthritis, of which ankylosing spondylitis is probably the most common.
If the latter is not the case, a connection can often be made with long periods of sitting on an uncomfortable surface, for example in the office. Then the complaints can usually be fought sustainably through a more appropriate choice of the lower surface of the seat and regular breaks from sitting with sufficient exercise.
Read more about the topic here: Inflammation of the nerves on the back.
Nerve inflammation from stress
Stress can definitely be an important factor in the development of nerve pain, but only in very few cases is it associated with nerve inflammation. However, this does not mean that those affected in the case of nerve pain attribute everything to excessive stress and neglect the symptoms. Because regardless of whether the stress is actually the cause or something else is behind the pain, the complaints are an alarm signal from the body. Therefore, those affected should always consult a doctor so that he can investigate which cause is triggering the symptoms.
diagnosis
If a patient suffers from the symptoms described above such as sensory disturbances, paralysis, etc., the Doctor-patient conversation seek the cause of a nerve inflammation by asking about the circumstances.
You will be asked about previous infections, trauma, medication, etc. With the neurological physical exam the symptoms are precisely recorded.
A Blood test serves to search for possible pathogens from a previous infection and for autoantibodies that can damage the nerve-enveloping tissue.
In addition, inflammation parameters can be checked.
The investigation of the Liquors (Cerebrospinal fluid) can be groundbreaking. This is taken by means of a lumbar puncture.
Special research methods
Depending on the nerve affected, there are other, very different examination methods to choose from. In the case of inflammation of the optic nerve, for example, it is examined by checking the pupillary light reflex, if there is a suspicion of inflammation of nerves on the arm, the muscle strength of the corresponding muscles is tested, etc.
Almost every nerve in the body can be examined according to its function.
Imaging methods such as MRI can be used to diagnose multiple sclerosis (MS) because they represent inflammatory sites in the central nervous system (CNS).
For example, the nerve conduction velocity can be measured using certain apparatus-based examinations.
This is determined in electroneurography. The conduction velocity of the nerves is slowed down when the myelin sheaths that surround the nerves are damaged.
Electromyography (EMG), in turn, in which the tension in the muscle is measured, can be used in the case of muscle dysfunction (such as flaccid paralysis) to determine whether the underlying problem is in the muscle or in the associated nerve.
Read more on the topic: Electromyography
If nerves of the autonomic nervous system are affected, the autonomous regulation of blood pressure, pulse, respiratory rate and digestion may be disrupted.
These disorders manifest themselves, for example, in heart problems, stomach cramps or constipation. The ECG, for example, is used for diagnosis (electrocardiogram).
Symptoms
In the case of nerve inflammation, the respective nerve can fail. So they can afferents Functions (conduction of excitations from the periphery to the central nervous system) such as the sensation of touch, temperature, vibration and pain and sensory perceptions such as taste, hearing, smell and balance may be disturbed.
This functional failure manifests itself in sensory disturbances (Paresthesia) such as “tingling”, “furry” or “electrifying feeling”, decreased or eliminated pain sensitivity, loss of vibration perception or decreased sensitivity to temperature perception. Are the efferents Functions (transmission of signals from the CNS to the periphery) are restricted, e.g. Motor nerve fibers that lead to the skeletal muscles no longer work properly. Symptoms are muscle weakness or paralysis.
If the vegetative / autonomous nervous system is affected, the transmission of information from the organs to the CNS is disturbed (pain sensation, chemical and mechanical stimuli), as is the regulation of smooth muscles (for example in the digestive tract or blood vessels), glands and heart muscles. Typical symptoms of disorders of the autonomic nervous system are blood pressure regulation disorders, heart problems or constipation.
Also read: These symptoms will help you recognize inflammation of the nerves
Pain
Most of those affected describe the pain of a nerve inflammation as burning, stabbing or tearing, and a tingling sensation often occurs. There are also reports of an electrifying nature of the pain.
Often the pain is reduced by physical activity and intensified at rest, which is also a good way of distinguishing between orthopedic causes for pain in the musculoskeletal system (e.g. joint arthrosis). Many sufferers benefit from heat and cold treatments and physiotherapy in terms of pain.