Kidney abscess
definition
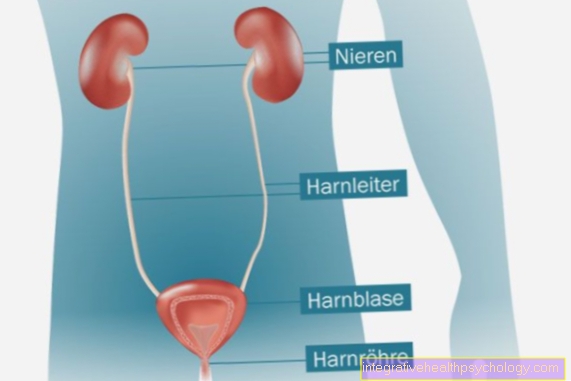
A kidney abscess is an encapsulated collection of pus between the surface of the kidney and what is known as the Gerota fascia. This is a type of skin that surrounds the kidney. This type of kidney abscess is also called a perinephritic abscess because it is located around the kidney. The paranephritic abscess is distinguished from this perinephritic abscess. This usually arises at the bottom of a perinephritic abscess. The pus breaks through the kidney capsule and is located in the so-called retroperitoneum, the space behind the kidney.

causes
There are different causes for the development of a kidney abscess.
- Renal infections, i.e. those affecting the kidneys, are an important possible cause of a kidney abscess Such an infection is also known as inflammation of the kidney pelvis (pyelonephritis). This is a bacterial, purulent infection that is often caused by inadequately treated bladder infections. The pathogens can climb up the ureter and infect the renal pelvis. Read also our topic: Pelvic inflammation
- Urine congestion, i.e. reduced outflow of urine, in the renal pelvis can lead to infections and ultimately to abscesses. Urinary congestion can have many reasons, such as obstruction of the drainage in the ureters due to tumors or paralysis.
- In addition to infections, tumors are also responsible for the development of a kidney abscess in some cases. Bacteria can settle in the disintegrated tumor tissue of a kidney tumor and thus also cause a kidney abscess. Read more on this topic at: Kidney cancer
People with a weakened immune system, drug addicts, patients in the intensive care unit or who need dialysis, and people with heart valve defects and bacterial infections of the heart valves are particularly at risk of developing a kidney abscess. All of these things increase the risk of bacteria spreading in various organs, including the kidney.
Symptoms
The so-called flank pain is typical of a kidney abscess. This is a lateral, roughly arched pain that is located a little below the lower edge of the shoulder blades. This flank pain can be extremely severe and is one-sided. The flank pain can continue to radiate to the abdomen or back. In this area, skin reddening can also be seen as a sign of inflammation. A large abscess can often be felt as a swelling under the skin. Typical symptoms are also fever, general fatigue and chills. The excretion of urine can be greatly reduced or even completely restricted, for example due to urinary congestion. Complications such as urosepsis or a rupture of the abscess can lead to a very acute clinical picture with organ failure and comatose states. Therefore, kidney abscesses should always be treated.
For more interesting information, read our topics: Kidney and flank pain
Symptoms of the spine
Kidney abscesses are located in close proximity to the spine and back. Depending on the size, there can even be swelling on the back next to the spine. Due to the pressure on surrounding structures, kidney abscesses often lead to radiating pain in the spine. In contrast to, for example, herniated discs or the like, kidney abscesses are characterized by other symptoms that are typical of an infection. These include fever, general fatigue, or nausea.
You might also be interested in this topic: Bump on the back - that's behind it!
diagnosis
A kidney abscess can be diagnosed using a variety of tests. The patient's medical history and symptoms already provide clues about the disease, which are then confirmed with further examinations. With the help of ultrasound, a kidney abscess can often be visualized. Other imaging tests, especially CT, are important to confirm the suspicion and to rule out other causes, such as tumors. The blood test reveals increased inflammation values such as CRP, procalcitonin and leukocytes. In addition, the so-called retention parameters of the kidneys deteriorate. These are urea and creatinine. The values rise because the kidneys can no longer excrete these substances well due to the abscess and their function is restricted. In a urine sample, germs are examined and resistance of the bacteria determined so that a suitable antibiotic therapy can be found.
Sonography
Sonography, also called ultrasound, is a simple and important diagnostic tool for identifying an abscess. In sonography, a so-called hypoechoic mass can be seen within the kidney capsule. It is called hypoechoic because it is darker than the surrounding tissue. Echogenic structures, however, are whiter. Whiter structures, i.e. more echogenic structures, can be seen in the abscess. These are air pockets. With a special examination, the Doppler sonography, the blood flow can be visualized. This is very useful to distinguish it from a tumor. Increased blood flow can only be seen at the edge of the abscess, whereas there is no blood flow inside the abscess.
therapy
A kidney abscess is always treated conservatively with antibiotic therapy. The antibiotics are given through the vein in the case of a kidney abscess. Antibiotic therapy can take place, for example, with amoxicillin and clavulanic acid and gentamicin or with so-called cephalosporins. The antibiosis is then adjusted depending on the pathogen diagnosis and determination of resistance. This determines which antibiotics the pathogens react to so that the right antibiotic can be selected. Depending on the course of the therapy and the defervescence of the person concerned, antibiotic therapy takes about 7 to 14 days. In the case of small abscesses with a diameter of less than 3 cm, conservative therapy is usually sufficient for treatment. Antipyretic and pain relieving drugs are used to accompany this. In the case of nausea and vomiting, antiemetics, i.e. drugs against vomiting, can also be administered. Larger abscesses, on the other hand, must also be treated interventionally or surgically, since conservative therapy alone is not sufficient.
You can find more interesting information at: Healing An Abscess - What To Look For!
surgery
Kidney abscesses that are larger than 3 cm in diameter must be treated interventionally or operated on. For abscesses between 3 and 5 cm, so-called percutaneous, retroperitoneal drainage of the abscess combined with antibiotic therapy is usually sufficient. During this treatment, the abscess is punctured and drained to the outside using a tube. The puncture is performed from the outside through the skin into the tissue and can be performed under local anesthesia. A sample of the emptied pus is always sent to the microbiology department for pathogen diagnosis. Abscesses larger than 5 cm may require multiple punctures or even an open surgical procedure. The abscess is surgically removed under anesthesia. In the case of a very large abscess and extensive kidney damage, it may even be necessary to remove the kidney to stop the inflammation.
Also read our topic: Surgery of an abscess
Duration of a kidney abscess
The duration of a kidney abscess differs from patient to patient. Most kidney abscesses develop rather subacutely, i.e. over several days to weeks, and not from one moment to the next. They often arise from pre-existing kidney diseases and infections. The treatment period for a kidney abscess usually lasts 2 to 3 weeks, which often require inpatient therapy. Treatment can last several weeks for complications such as urosepsis.
Abscess in the abdomen
A dreaded complication of kidney abscess is a breakthrough through the so-called Gerota fascia. This type of capsule surrounds the kidney and separates it from the retroperitoneal space, a space in the body that contains various organs such as the kidney, pancreas and parts of the intestine. When the pus is emptied into this space, inflammatory reactions and blood poisoning (sepsis) can occur. Antibiotic therapy and often surgical removal of the abscess are essential in this case.
Read more on this topic at: Abscess in and on the abdomen - how dangerous is it?