Giant cell arteritis
Synonyms
Temporal arteritis, cranial arteritis, Horton's arteritis, Horton's disease
definition
The Giant cell arteritis belongs to the inflammatory diseases of the blood vessels. It belongs to the group of rheumatic diseases (rheumatism). Only affected are aorta and Arteriesbut not veins or capillaries. (Hence the name arteritis = inflammation of the arteries.)

A distinction is made between two different forms:
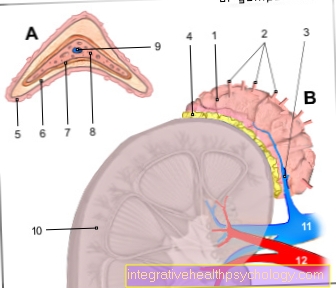
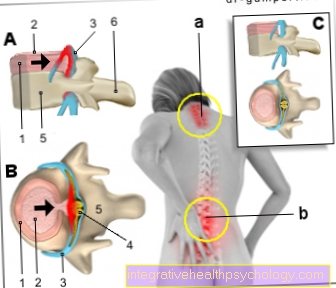
- The classic shape represents inflammation of the outside on head temporal artery (lat. A. temporalis). Typically, the whole of the clavicle region is drawn into the head Carotid artery (lat. Carotid artery) and the branching arteries are involved in the inflammatory process. Leg arteries or arteries of the bowels can also rarely be affected.
- One form preferentially affects the one aorta and their large branches.
Epidemiology
The disease mostly affects older patients over 50 years of age.
Women are more often affected than men.
With around 30 new cases per year under 100,000 inhabitants, giant cell arteritis is the most common inflammation of the vessels (Vasculitis). It occurs particularly often in combination with rheumatic diseases (rheumatism) on.
causes
The cause of giant cell ateritis (ateritis temoralis Horton) is largely unknown. It is possible that predisposition (genetic disposition) plays a role. There is a connection with diseases in which the immune system is directed against the own body (autoimmune diseases = rheumatism; cf. Greek autos = self). The outbreak of the disease is favored by previous bacterial or viral damage to the vessels.
Symptoms
The main symptoms are headaches. The temporal artery on skull is thickened (visible from the outside) and very sensitive to pressure.in most cases only one side of the skull is affected, occasionally both the left and right sides are affected. Generally there is a strong feeling of illness with exhaustion, possibly. Fever, depression, Loss of appetite and weight loss. In addition, signs of inflammation can be detected in the blood (increased erythrocyte sedimentation rate (ESR) and the C reactive protein (CRP)).
Further complications arise as the disease progresses: Infestation of the das eye supplying artery (arteria ophtalmica) can lead to the occlusion of the vessel. Then the eye (especially the one for a Visual impression indispensable retina) no longer or insufficiently supplied with blood. The consequences range from impaired vision to Blindness (in about half of all sick people).
Patients over 65 years of age often experience additional symptoms in the form of shoulder pain and / or morning limb stiffness (which is known as Polymyalgia rheumatica referred to as). The reason is an accompanying inflammation of the connective tissue lining the joints from the inside (the synovia, the inflammation is therefore called synovitis).
Disease emergence
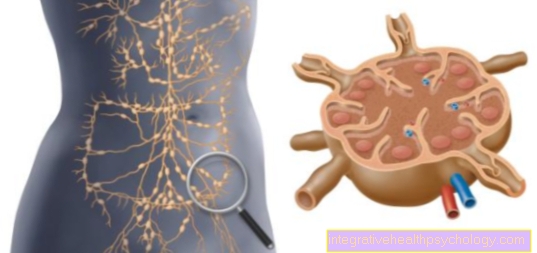
The inflammatory destruction of the vessels occurs in two different ways, for which the own immune system is responsible: On the one hand, defense cells (white blood cells, large leukocytes) form proteins (so-called antibodies) that attach to the structures of the vessels and then start a chain reaction set in which various endogenous cells as well as enzymes and messenger substances (mediators) that destroy the blood vessels are involved (so-called immune reaction type II). So-called giant cells are typically involved in the inflammation (hence the name), which can be detected by microscopic examination of the affected vessels (see below).
The second possibility of vascular damage is the undesired connection of the proteins formed by overreacting immune cells with the body's own structures (antigens) floating in the blood. These compounds are called immune complexes and also set the destructive chain reaction in motion. In both cases, the result is damage to the
- inner (called intima) vascular layers and
- the middle layer (media) made up of small, specialized muscle cells.
In addition, the elastic membrane breaks into pieces between the two layers of the vessel wall. These characteristic vascular changes facilitate the clear determination (if the clinical symptoms are insufficient) of giant cell arteritis (Horton's disease) when viewing tissue samples with a microscope. However, the clear detection of existing vascular changes is easier than the reliable exclusion of a disease, since the entire vessel does not have to be affected. Then the material of the tissue sample is apparently healthy and inconspicuous, because an unaffected part of the vessel was accidentally removed (so-called skip lesions). To avoid this, pieces of vessels more than two centimeters long are often removed.
First indications of a giant cell arteritis (Horton's disease) with narrowing of the vessels can also be an ultrasound examination (sonography). The thickness of the vessels can be determined during an ultrasound examination. Especially with large vessels, the thickness of the vessel wall can be determined to the millimeter. A covered vessel wall in the ultrasound examination can indicate Horton's disease. However, other vascular diseases, such as hardening of the arteries, can also cause the vascular wall to thicken.
diagnosis
To secure the diagnosis, the Ultrasound examination or one Magnetic resonance imaging of the head (MRI of the head). Magnetic resonance sonography can also be used to visualize the inflamed, changed and hidden vessel wall.
A clear diagnosis of giant cell lateritis can only be made with a sample of the inflamed vessel (biopsy) and a histological (tissue) examination.
Further references to a Horton's disease the blood test with increased inflammation values and, if necessary, evidence of rheumatism - typical changes in the blood / Laboratory values (e.g. rheumatoid factors or antinUkrainian A.ntibodies (ANA)) give.
therapy
The disease is serious, so therapy should be started immediately if the typical symptoms are suspected in order to prevent the disease from progressing. High-dose corticosteroids (Cortisone), which are supposed to contain the inflammation. When it improves, the dose is then slowly reduced and continued for a year or two in as low a dose as possible. Alternatively, the corticoisteroids (cortisone) can be completely or partially replaced by immunosuppressants (e.g. Methotrexate) be replaced.
forecast
Without therapy, 30% of those affected go blind. If therapy is started immediately and carried out consistently, almost all patients can be free of symptoms.
Chronic precursors are an exception.