Esophageal diverticulum
Synonyms
Zenker's diverticulum, pulsation diverticulum, traction diverticulum, hypopharyngeal diverticulum, cervical diverticulum, esophageal sac
Medical: esophageal diverticulum
English: diverticel
definition
As Diverticulum denotes congenital or acquired protrusions of wall parts of a hollow organ (esophagus, Intestines, bladder). Diverticula can be found throughout Digestive tract occurrence. They are most often found in the colon (diverticulosis), but also in the esophagus are they to be found.
An esophageal diverticulum is the term used to describe a sagging of the esophageal wall. A distinction is made between different forms of diverticulum, depending on which layers of the esophageal wall are involved in the formation of the diverticulum. Be differentiated Traction diverticulum ("Real" diverticula) and Pulsation diverticulum ("False" diverticula).
Epidemiology
The esophageal diverticulum (esophageal diverticulum) is a rare disease, but the risk of developing the disease increases with age. 80% of those affected are men, two thirds of whom are older than 70 years.
The most common diverticulum is Zenker's diverticulum with approx. 70%, followed by parabrochial diverticula with approx. 21%. Epiphrenal diverticula are less common in about 9% of cases.
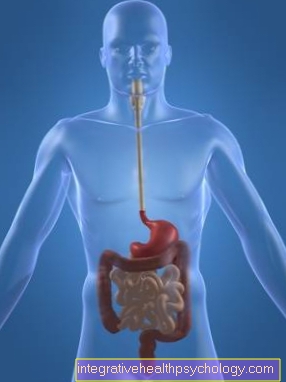
Figure esophagus

- esophagus
(Neck section) -
Esophagus, pars cervicalis - Nasal cavity - Cavitas nasi
- Oral cavity - Cavitas oris
- Windpipe (approx. 20 cm) - Trachea
- esophagus
(Chest section) -
Esophagus, pars thoracica - esophagus
(Abdominal section) -
Esophagus, pars abdominalis - Stomach entrance -
Cardia - Stomach body -
Corpus gastricum - Throat -
Pharynx - Thyroid -
Glandula thyroidea
You can find an overview of all Dr-Gumpert images at: medical illustrations

Normal course of the esophagus
Normal esophagus with transition to the stomach

Esophageal diverticulum
- Diverticulum
- Esophagus (esophagus)
- Stomach (gaster)
At the real diverticulum (Traction diverticulum) there is a protuberance of all esophageal wall layers. This shape is created by a pull (traction) from the outside on the esophageal wall. Especially in the area of the fork windpipe (Tracheal bifurcation) and the large main bronchi (branches of the windpipe), this form of diverticulum can arise. That's why they are also called Parabronchial diverticulum (= diverticula lying next to the branches of the ventilation duct). The causes for the development of tensile diverticula are different:
During embryonic development (the period of prenatal development in humans), remnants of tissue bridges can remain between the esophagus and the windpipe and thus create a pull on the esophageal wall. This means that the esophagus does not separate completely from the windpipe.
A scar train, e.g. after a lymph node inflammation (Lymphadenitis), can lead to the development of a traction diverticulum (non-specific inflammation, tuberculosis). These scars lead to the esophageal wall being drawn outwards in the shape of a lobe or a funnel. Such diverticula are mostly incidental, small and usually do not cause any symptoms.
In contrast to the traction diverticulum, this is false diverticula (pulsation or pseudodiverticulum) often associated with discomfort for the patient. The pulsation diverticulum arises as a result of weak points in the muscle wall of the esophagus. During the act of swallowing, the muscle contraction of the esophagus and the conveyance of the food cause an increase in pressure in the esophagus, as a result of which parts of the mucous membrane (mucosa and submucosa) can turn outwards through a muscle gap in the esophageal wall. It can be said that there is a mismatch between the pressure in the esophagus and the stability of the muscle wall.
This also belongs to the pulsation diverticula Zenker's diverticulum. The Zenker's diverticulum (named after the pathologist Friedrich A. von Zenker 1825-1898) is the most common diverticulum of the esophagus with 70% and is located just above the esophageal mouth (esophageal entrance in front of the stomach) in the lower posterior wall of the pharynx (Hypopharynx). This is also known as the muscle weak point typical of Zenker's diverticulum Killian's triangle. This is a regularly created weak point in the esophageal wall, which is why a particularly large number of pulionic diverticula develop in this area. Another assumption is that there is a dysfunction of the upper esophageal sphincter (esophageal mouth). This dysfunction leads to an increase in pressure on the Kilian muscle gap, which leads to the formation of diverticula.
In approx. 10% of the cases the pulsation diverticula are located shortly before the passage of the esophagus through the diaphragm into the abdomen (Abdomen). They are called there Epiphrenal diverticula (above the diaphragm lying diverticula). This diverticulum can be caused by a strong lower esophageal sphincter (lower esophageal sphincter), which can cause food to jam, increasing pressure on the esophageal wall in that area. The epiphrenic diverticulum can reach a considerable size. Accordingly, complaints are also caused more frequently.
In rare cases, an esophageal diverticulum can develop as a result of an esophageal tumor or an overactive esophageal muscle (hypercontractile esophagus).
Complications
The following complications can occur as a result of diverticular disease of the esophagus:
- The enclosed food can serve as a breeding ground for germs (bacteria). This can lead to inflammation of the lining of the esophagus (esophagitis). The inflammatory processes can in turn cause bleeding of the esophageal lining. If changes in the esophageal tissue occur due to chronic inflammation, tubular infectious ducts, so-called fistulas, can develop, which can establish a connection to neighboring structures, in particular to other hollow organs.
- The re-burping of food residues can lead to inhalation of these food residues (aspiration), especially at night. This can lead to repeated (recurrent) severe pneumonia (aspiration pneumonia) and pus ulcers in the lungs (lung abscess).
- In very rare cases, overstretching the diverticulum can lead to a tear (rupture) in the diverticulum wall. This enables porridge to pass through into the chest. This can cause life-threatening inflammation of the middle layer (mediastinitis).
- Patients with an esophageal diverticulum also have an increased risk of developing a malignant (malignant) tumor in the esophagus (esophageal carcinoma). The chronic irritation of the esophageal mucous membrane can initiate remodeling processes in the tissue, which in the worst case can lead to the development of tumors.
diagnosis
X-ray - swallow of porridge:
During this examination, the esophagus is X-rayed while the patient swallows an X-ray contrast agent. The contrast agent is placed on the esophageal wall, whereupon it is accessible for assessment. Characteristic of diverticular disease is the appearance of a contrast medium-filled round to sac-shaped esophageal protuberance.
Note
Water-soluble contrast media should be used in patients with severe swallowing disorders and who have already had aspiration pneumonia
Are used because there is a particularly high risk of aspiration (inhalation) of the contrast medium into the lungs. If a non-water-soluble contrast medium were to get into the lungs, this would result in a foreign body reaction that is difficult to treat (reaction of the body to the contrast medium) and inflammation of the lung tissue.
Dynamic video fluoroscopy (radiological examination of swallowing):
This examination method is significantly less X-ray stressful and more meaningful than the classic X-ray swallow.
With a digital camera, the esophagus is filmed and recorded during the act of swallowing. Diverticular bulges and above all Movement disorders of the esophagus during the act of swallowing can be easily diagnosed. Another advantage is that in the assessment of esophageal movement disorders during repeat examinations, comparisons with previous recordings are possible and the progress of therapy can be documented.
Esophagomanometry (measurement of pressure in the esophagus):
A thin tube (catheter) is first placed through the nose into the stomach and then slowly pulled back towards the mouth, whereby the patient has to swallow some water regularly. When the catheter is withdrawn, the internal esophageal pressure is continuously measured at the end of the catheter. A computer graphic shows the pressure conditions in the course of the esophagus. Functional disorders of the esophagus can thus be diagnosed.
With this examination, functional disorders of the esophagus can be detected, as they can occur in the area of the lower esophageal sphincter in the context of epiphrenal diverticulum development. Since there is no internal pressure increase in the esophageal wall as the cause of the development of parabronchial traction diverticula, the examination of this type of diverticulum is not conclusive
Endoscopy (esophagogastroscopy):
The "mirroring" (Endoscopy) of the esophagus is not a standardized procedure for diagnosing a diverticulum. It is used if there are still ambiguities in the previous examinations (confirmation of diagnosis, exclusion of tumor), complications need to be assessed (inflammation) or a tissue sample (biopsy) is required. At a Gastroscopy a flexible tube camera (endoscope) is “swallowed” by the patient during light anesthesia, which then transmits images of the inside of the esophagus and stomach to a monitor. The most common reason for an endoscopy to be performed is to rule out an esophageal tumor.
In the case of diverticular disease, the mirror must be carried out particularly carefully because the diverticulum wall is not very stable and can easily be pierced with the endoscope.