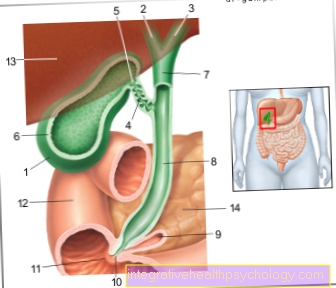
Colpitis - the inflammation of the vagina
introduction
As colpitis or also Vaginitis is called a vaginal infection. Colpitis can have different causes and is therefore also divided into different forms. For example, there are primary, secondary and atrophic colpitis, the latter mainly occurring in old age due to a lack of female sex hormones.

Colpitis is a common disease overall. Most women will develop colpitis at least once in their life. Since the acidic vaginal environment is important to keep pathogens away from the uterus and thus also the rest of the body, it is important that colpitis is adequately treated. In this way, the worse complications of progressive colpitis can be prevented.
Senile colpitis occurs acutely after menopause. Find out more about this at:
Senile colpitis - what can you do about it?
Forms of colpitis
In colpitis, different forms are distinguished depending on the cause:
- Primary colpitis: Primary colpitis develops due to a high bacterial load in the vaginal environment. Primary means that the vaginal environment itself was intact, but is now being attacked and damaged by the pathogens and an infection manifests itself on this soil.
- Secondary colpitis: Secondary colpitis develops as a result of an initially present disturbance of the vaginal flora. The vaginal lining is already attacked before the infection develops. Due to the reduced barrier, pathogens can now multiply better and secondary to inflammation of the vaginal mucous membrane.
A special form of secondary colpitis is atrophic colpitis, which is characterized by a lack of female sex hormones (Estrogens) manifested.
In old age (after the menstrual period has ceased) there is a reduced production of estrogens. However, these are essential for maintaining the acidic vaginal environment and the barrier function of the vaginal mucosa. Therefore, vaginal infections can develop more quickly and easily in older women. The same applies to girls who have not yet started their menstrual period. They too do not have a sufficiently high level of estrogen that could create optimal resistance of the vaginal environment.
causes
Basically, colpitis can easily develop if there is a disorder of the natural vaginal flora. If this normally acidic environment is attacked, pathogens can multiply more easily and lead to an infection. The vaginal flora can be influenced by different factors. These include, for example, drugs (especially antibiotics), as these unbalance the natural and useful bacterial flora of the vagina, and tampons, which dry out the vaginal mucous membrane and thus make it more vulnerable. Excessive intimate hygiene in the form of very frequent washing and the use of alkaline soaps in the intimate area can also promote colpitis. The same applies to vaginal douching. Last but not least, patients who have diabetes mellitus also suffer more frequently from vaginal infections. The reason is that these patients often excrete more sugar with the urine and the bacteria and also fungi in the intimate area feed on this sugar. This forms a good basis for their multiplication and, consequently, for the development of colpitis.
Please also read our page about Vaginal thrush or vaginal inflammation
Lack of estrogen
Over time, the woman's estrogen level continues to decline. Especially during the menopause there is an abrupt drop in the hormone. Estrogen not only regulates the female cycle, but also promotes the growth and renewal of the vaginal mucosa. If the estrogen level falls, the mucous membrane is less supplied with blood, it contracts, becomes dry and can easily tear when touched. Itching and burning are the first consequences of the changes in the mucous membrane (atrophy). Through the thin, cracked mucous membrane, bacteria and fungi can easily migrate into the mucous membrane, spread and cause inflammation.
Read more on the subject at: Menopause symptoms
Colpitis pathogen
Ultimately, it is the various pathogens that cause colpitis. The spectrum of pathogens is very mixed. It is often different pathogens at the same time that cause the infection.
Most frequently (about 40% of the cases) however, there is an infection with the bacterium Gardnerella vaginalis. Fungal infections of the vagina follow in 20% of cases, for example with the yeast Candida albicans. 10% of colpits are caused by colonization with the parasite Trichomonas vaginalis, another 10% by chlamydia, which also belong to the bacteria.
The remaining vaginal infections are caused by mixed infections or other pathogens, for example by human papilloma viruses (HPV) caused. Human papillomaviruses are transmitted through sexual intercourse and can lead to the formation of genital warts in the genital area (Condylomata acuminata) to lead. HPV 16 and 18 subtypes are also associated with the development of cervical cancer (Cervical cancer) associated. Herpes viruses (HSV) can cause vaginal inflammation and general inflammation of the genital area.
Symptoms
The main symptom of colpitis is vaginal discharge. However, since a healthy woman can also have vaginal discharge, the abnormal discharge must be differentiated from normal discharge as part of the normal cycle. The discharge that occurs in colpitis is usually changed in color. It can be yellowish, greenish, white or transparent. The consistency is often crumbly, especially with fungal infections. In the case of fungal infections, there is usually no odor development, while a fishy, unpleasant odor can occur with a bacterial vaginal inflammation.
When infected with Trichomonas vaginalis, the discharge is often frothy, yellowish, and causes a severe burning sensation in the vagina.Infection with herpes viruses in the genital area, on the other hand, is usually noticed by small, painful blisters that are often grouped around the entrance of the vagina. In addition to changes in discharge, colpitis can also have other symptoms. Many women complain of pain during intercourse (Dyspareunia) or a burning sensation in the vagina. An excruciating itch is also very common. This occurs especially with fungal infections. However, infection with human papillomavirus (HPV) usually does not cause any symptoms as long as genital warts do not appear. However, these can cause abnormal sensations in the genital area.
Read more about this under: Burning in the genital area- causes and treatment
diagnosis
The diagnosis of colpitis is made as part of a gynecological examination. In the case of visible skin changes, for example genital warts or cold sores, the diagnosis is often only made based on the clinical picture. Otherwise, a vaginal smear is taken, which can be examined under the microscope. The pathogens become visible. Depending on the pathogen, various smears and laboratory tests can be requested. The sensitivity of the pathogens to various antibiotic agents can also be determined in the laboratory, so that the doctor can find out which antibiotics he can use effectively against the pathogens.
A chlamydial infection can also be determined by examining your urine. Fungal infections can often be seen on the vaginal mucous membrane with the naked eye. Depending on the findings, the attending physician can then initiate the appropriate therapy.
therapy
The therapy of colpitis depends on the respective pathogen. Antibiotics are usually given if you have a bacterial infection. Fungal infections are treated with antifungal drugs. Vaginal suppositories are often used, which have to be inserted into the vagina every day for a few days. In this case, the therapy is usually combined with a cream to be applied externally, so that fungi that are externally in the genital area are also killed.
It is important that the treatment of the sexual partner is also considered. This is especially true if unprotected sexual intercourse was practiced at the time of infection. Otherwise there is a risk of mutual re-infection. In addition, after treatment of the colpitis, a cause research should be carried out and risk factors for further colpitis should be eliminated. Building a healthy vaginal environment is crucial for this. For example, the use of lactic acid bacteria (Döderlein bacteria) be advisable. These can be inserted into the vagina in the form of capsules and build up the healthy vaginal flora there.
These drugs are used
The drug therapy depends on the causative pathogens. The antibiotic metronidazole is often used for bacterial infections. It works primarily against bacteria, which grow best without oxygen (anaerobic bacteria) and are common in the vagina. If there are other bacteria in the infection, e.g. Gonococci, basically the antibiotic must be adjusted accordingly and changed to ceftriaxone. The antimycotic clotrimazole works against fungal infections.
Depending on the severity of the infection, the drugs can be used locally as suppositories or systemically as tablets. In addition, antiseptics such as Betaisadona are sometimes prescribed for topical use. If it is a sexually transmitted disease, the partner must always be treated in order to avoid the so-called ping-pong effect.
These home remedies can help
The cause of inflammation and infection of the vaginal mucosa is a changed vaginal environment. Usually acidic conditions prevail here with a pH value of 4-5. If the pH changes, bacteria can settle more easily. There are a number of home remedies that may help bring the pH back down. These include yoghurt and milk, which create an acidic environment due to the lactic acid bacteria they contain. There are also home remedies, such as black tea and garlic, that are believed to have antibacterial properties.
In addition, Sitz baths with apple cider vinegar - also lowering the pH value, or tea tree oil (antibacterial) can be carried out. In addition, fenugreek seeds can be infused with hot water or mixed with yogurt to drink. Despite everything, it must be emphasized that none of these home remedies has been proven to be medicinally effective. The introduction of substances such as milk or garlic can additionally irritate the mucous membrane and also worsen the inflammation. Those affected should definitely consult a doctor and discuss possible therapy options.
Complications
If colpitis is not treated early enough or adequately, complications can develop. Due to the disturbed vaginal environment, pathogens can spread into the uterus and from there via the fallopian tubes to the ovaries and into the abdominal cavity. The consequences are, for example, uterine inflammation, fallopian tube inflammation or ovarian inflammation (Adnexitis), and in the worst case inflammation of the peritoneum (Peritonitis) with secondary blood poisoning. In pregnant women in particular, colpitis is a very serious disease, as it can lead to premature birth if left untreated. Existing infections can pass to the child during birth and lead to various complications. This is especially true for infections with herpes viruses, gonococci and chlamydia. In such a case, it is not uncommon for the child to be delivered by caesarean section in order to avoid a child's infection.
forecast
As a rule, colpitis can be treated well. If the pathogen is known, a targeted therapy be initiated. During therapy, it should be noted that it is carried out regularly and completely in order to really eliminate all pathogens. In this way, colpitis is mostly survived within a few daysas long as it was recognized and treated early on.
prophylaxis
The best prophylaxis to avoid colpitis is to build up a healthy vaginal flora. To prevent the transmission of pathogens through sexual partners, a condom should be used during sexual intercourse. In addition, proper intimate hygiene should be practiced. Too infrequent, but also too frequent, washing of the genital area increases the risk of developing colpitis. In addition, no soaps, shampoos or vaginal douches should be used.
Furthermore, it can have a preventive effect to wipe the anus from front to back after defecation so that intestinal bacteria are not wiped forward towards the vaginal opening. In women who develop colpitis more often, lactic acid bacteria can help keep the vaginal flora healthy. Lactic acid bacteria are available in capsule form from pharmacies. As a prophylactic, they can be inserted into the vagina once a week, where they maintain the acidic environment that prevents pathogens from multiplying. Nevertheless, vaginal inflammation can occur even if these general behavioral measures are observed. However, if you see a gynecologist in good time, the disease can usually be treated well and safely.
Colpitis During Pregnancy - You Must Know That!
Colpitis during pregnancy can cause serious complications and must definitely be treated. Infections from the vagina can lead to infections of the uterus and the unborn child. Depending on the pathogen, it can lead to undesirable developments or even death of the child. In addition, premature labor and thus premature birth can be triggered. A caesarean section is usually performed in patients with existing colpitis at the time of birth, as the child can become infected with the bacteria on the way through the birth canal and vagina. In the womb, the child is partially protected by the mother's immune system. After the birth, however, the child's immune system is significantly weakened. Bacterial infections can therefore lead to serious illnesses.
Read more on the subject at: Diseases in Pregnancy
What is atrophic colpitis?
Athrophic colpitis is usually a symptom of old age. The falling estrogen level during menopause makes the vaginal lining thin, cracked and dry. This encourages bacteria to enter and inflammation to develop. Menopausal women often report vaginal itching and burning or painful intercourse. As a result of this changed vaginal environment, germs can settle and cause inflammation. Therapy should therefore be initiated at the first signs of vaginal dryness in order to prevent infection early. Moisturizing gels with hyaluronic acid, as well as vitamins A and E or, if necessary, ointments containing estrogen can be used here.
Read more on the subject at: Vaginal dryness